16 Contemporary Topics: Human Biology and Health
Joylin Namie, Ph.D., Truckee Meadows Community College
This chapter is a revision from “Chapter 16: Contemporary Topics: Human Biology and Health” by Joylin Namie. In Explorations: An Open Invitation to Biological Anthropology, first edition, edited by Beth Shook, Katie Nelson, Kelsie Aguilera, and Lara Braff, which is licensed under CC BY-NC 4.0.
Learning Objectives
- Describe the major transitions in patterns of disease that have occurred throughout human evolution.
- Describe what is meant by a “mismatch” between our evolved biology and contemporary lifestyles and how this is reflected in modern disease patterns.
- Explain how the human stress response can positively and negatively have an impact on health.
- Explain what a “syndemic” is and why the COVID-19 pandemic represents one.
- Describe the ways institutionalized racism and bias in the medical field contributed to different rates of exposure, differential treatment, morbidity, and mortality from COVID-19 for different ethnic groups in the United States.
When was the last time you needed to do research for an upcoming paper? I bet you started by looking for information online. How did you go about your search? Which websites looked promising? Which ones did not entice you to click past the home page? Once you found one you thought might be useful, how much time did you spend searching for information? At what point did you decide to leave that site and move on? I would wager money that you never once thought your behavior had anything to do with human evolution, but it does.
Although we may not often stop to think about it, our evolutionary past is reflected in many aspects of modern life. The ways we “forage” for information on the internet mimics the ways we once foraged for food during our several-million-year history as hunter-gatherers (Chin et al. 2015). Humans are visual hunters (Lieberman 2006). We practice optimal foraging strategy, meaning we make decisions based on energy return for investment (McElroy and Townsend 2009). When we search for information online, we locate a “patch,” in this case a website or research article, then quickly scan the contents to discern how much of it is useful to us. Like our hominin ancestors, we spend more time in “patches” with abundant resources and abandon sites quickly once we have exhausted the available goods. As with internet searches, our evolutionary past is also reflected in the kinds of landscapes we find appealing, the foods that taste good to us, why we break a sweat at the gym, and why we have to go to the gym at all (Bogin 1991; Dutton 2009; Lieberman 2015). Many of the health problems facing humans in the 21st century also have their beginnings in the millions of years we roamed the earth as foragers.
This chapter addresses contemporary health issues from an evolutionary perspective. It begins with a review of diet, activity patterns, and causes of morbidity (sickness) and mortality (death) among our preagricultural ancestors, which form the foundation for the ways our bodies function today. This is followed by a brief review of the health consequences of the transition to agriculture (see “Cultural Effects of Agriculture” in Chapter 12 for more detail), marking the first of several major epidemiological transitions (changes in disease patterns) experienced by humankind. It then addresses health conditions affecting modern, industrialized societies, including obesity, diabetes, heart disease, cancer, and the effect of stress on health. The environments in which we now live and the choices we make put a strain on biological systems that came about in response to selective pressures in our past, meaning the ways our bodies evolved are, in many ways, a mismatch for the conditions of modern life.
Preagricultural Humans
Diet
Humans may be the species with the longest list of nutritional requirements (Bogin 1991). This is due to the fact that we evolved in environments where there was a high diversity of edible species but low densities of any given species. Homo sapiens sapiens require 45–50 essential nutrients for growth, maintenance, and repair of cells and tissues. These include protein, carbohydrates, fats, vitamins, minerals, and water. As a species, we are (or were) physically active with high metabolic demands. We are also omnivorous and evolved to choose foods that are dense in essential nutrients. One of the ways we identified high-calorie resources in our evolutionary past was through taste, and it is no accident that humans find sweet, salty, fatty foods appealing.
The human predisposition toward sugar, salt, and fat is innate (Farb and Armelagos 1980). Receptors for sweetness are found in every one of our mouth’s 10,000 taste buds (Moss 2013). Preference for sweet makes sense in an ancestral environment where sweetness signaled high-value resources like ripe fruits. Likewise, “the long evolutionary path from sea-dwelling creatures to modern humans has given us salty body fluids, the exact salinity of which must be maintained” (Farb and Armelagos 1980), drawing us to salty-tasting things. Cravings for fat are also inborn, with some archaeological evidence suggesting that hominins collected animal bones for their fatty marrow, which contains two essential fatty acids necessary for brain development (Richards 2002), rather than for any meat remaining on the surface (Bogin 1991).
Bioarchaeological studies indicate Paleolithic peoples ate a wider variety of foods than many people eat today (Armelagos et al. 2005; Bogin 1991; Larsen 2014; Marciniak and Perry 2017). Foragers took in more protein, less fat, much more fiber, and far less sodium than modern humans typically do (Eaton, Konner, and Shostak 1988). Changes in tooth and intestinal morphology illustrate that animal products were an important part of human diets from the time of Homo erectus onward (Baltic and Boskovic 2015; Richards 2002; Wrangham 2009). Once cooking became established, it opened up a wider variety of both plant and animal resources to humans. However, the protein, carbohydrates, and fats preagricultural peoples ate were much different from those we eat today. Wild game lacked the antibiotics, growth hormones, and high levels of cholesterol and saturated fat associated with industrialized meat production today (Walker et al. 2005). Wild game was also protein dense, providing only 50% of energy as fat (Lucock et al. 2014). The ways meat is prepared and eaten today also have implications for disease.
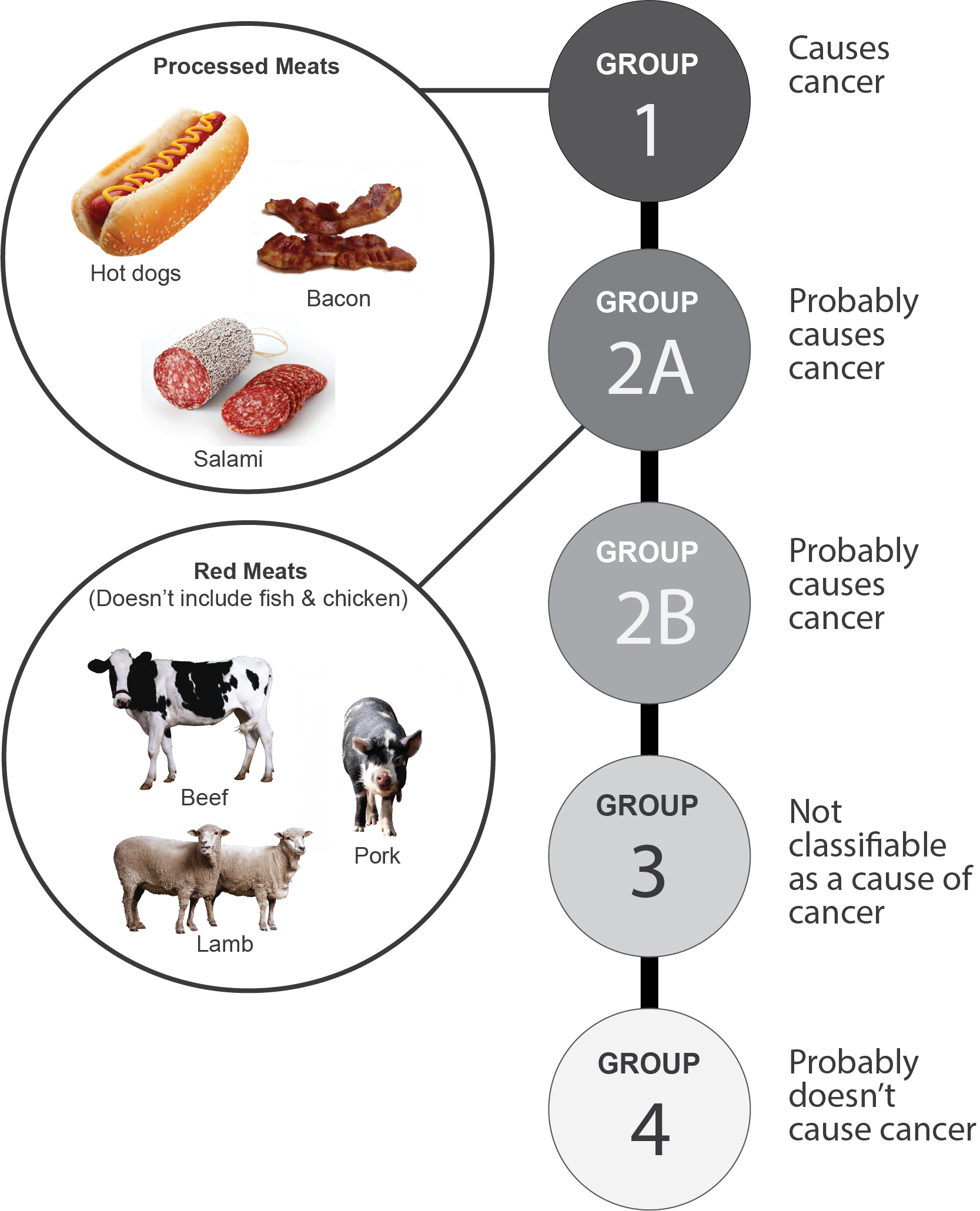
Meats cooked well done over high heat and/or over an open flame, including hamburgers and barbecued meats, are highly carcinogenic due to compounds formed during the cooking process (Trafialek and Kolanowski 2014). Processed meats that have been preserved by smoking, curing, salting, or by adding chemical preservatives such as sodium nitrite (e.g., ham, bacon, pastrami, salami, and beef jerky) have been linked to cancers of the colon, lung, and prostate (Abid, Cross, and Sinha 2014; Figure 16.1). Nitrites/nitrates have additionally been linked to cancers of the ovaries, stomach, esophagus, bladder, pancreas, and thyroid (Abid, Cross, and Sinha 2014). In addition, studies analyzing the diets of 103,000 Americans for up to 16 years indicate that those who ate grilled, broiled, or roasted meats more than 15 times per month were 17% more likely to develop high blood pressure than those who ate meat fewer than four times per month, and participants who preferred their meats well done were 15% more likely to suffer from hypertension (high blood pressure) than those who ate their meats rare (Liu 2018). A previous study of the same cohort indicated “independent of consumption amount, open-flame and/or high-temperature cooking for both red meat and chicken is associated with an increased risk of type 2 diabetes among adults who consume animal flesh regularly” (Liu et al. 2018). Although meat has been argued to be crucial to cognitive and physical development among hominins (Wrangham 2009), there has been an evolutionary trade-off between the ability to preserve protein through cooking and the health risks of cooked meat and chemical preservatives.
Although carbohydrates represent half of the diet on average for both ancient foragers and modern humans, the types of carbohydrates consumed are very different. Ancient foragers ate fresh fruits, vegetables, grasses, legumes, and tubers, rather than the processed carbohydrates common in industrialized economies (Moss 2013). Their diets also lacked the refined white sugar and corn syrup found in many modern foods that contribute to the development of diabetes (Pontzer et al. 2012).
Physical Activity Patterns
How do we know how active our ancestors were? Hominin morphology and physiology provide us with clues. Adaptations to heat discussed in Chapter 14 evolved in response to the need for physical exertion in the heat of the day in equatorial Africa. Human adaptations for preventing hyperthermia (overheating) suggest an evolutionary history of regular, strenuous physical activity. Research with modern foraging populations also offers clues to ancient activity patterns. Although subject to sampling biases and marginal environments (Marlowe 2005), modern foragers provide the only direct observations of human behavior in the absence of agriculture (Lee 2013). From such studies, we know foragers cover greater distances in single-day foraging bouts than other living primates, and these treks require high levels of cardiovascular endurance (Raichlen and Alexander 2014). Recent research with the Hadza in Tanzania indicates they walk up to 11 kilometers (6.8 miles) daily while hunting and gathering (Pontzer et al. 2012), engaging in moderate-to-vigorous physical activity for over two hours each day—meeting the U.S. government’s weekly requirements for physical activity in just two days (Raichlen et al. 2016; Figure 16.2). The fact that humans were physically active in our evolutionary past is also supported by the fact that regular physical exercise has been shown to be protective against a variety of health conditions found in modern humans, including cardiovascular disease (Raichlen and Alexander 2014) and Alzheimer’s dementia (Mandsager, Harb, and Cremer 2018), even in the presence of brain pathologies indicative of cognitive decline (Buchman et al. 2019).

Infectious Disease
Population size and density remained low throughout the Paleolithic, by some estimates only 0.4 inhabitants per square kilometer (McClellan and Dorn 2006). This limited morbidity and mortality from infectious diseases, which sometimes require large populations to sustain epidemics. Our earliest ancestors had primarily two types of infections with which to contend (Armelagos 1990). The first were organisms that adapted to our prehominin ancestors and have been problems ever since. Examples include head lice, pinworms, and yaws. A second set of diseases were zoonoses, diseases that originate in animals and mutate into a form infectious to humans. One example is the Human Immunodeficiency Virus (HIV) that originated in nonhuman primates and was likely passed to humans through the butchering of hunted primates for food (Sharp and Hahn 2011). Zoonoses that could have infected ancient hunter-gatherers include tetanus and vector-borne diseases transmitted by flies, mosquitoes, fleas, midges, ticks, and the like. Many of these diseases are slow acting, chronic, or latent, meaning they can last for weeks, months, or even decades, causing low levels of sickness and allowing victims to infect others over long periods of time. Survival or cure does not result in lasting immunity, with survivors returning to the pool of potential victims. Such diseases often survive in animal reservoirs, reinfecting humans again and again (Wolfe et al. 2012). A study of bloodsucking insects preserved in samples of amber dating from 15 to 100 million years ago indicates that they carried microorganisms that today cause diseases such as river blindness, typhus, Lyme disease, and malaria (Poinar 2018). Such diseases may have been infecting humans throughout our history and may have had significant impacts on small foraging communities because they more often infected adults, who provided the food supply (Armelagos et al. 2005).
Health
Given their diets, levels of physical activity, and low population densities, nomadic preagricultural humans were likely in better health than many modern populations. This assertion is supported by comparative research conducted with modern foraging and industrialized populations. Measures of health taken from 20th-century foraging populations demonstrate excellent aerobic capacity, as measured by oxygen uptake during exertion, and low body-fat percentages, with triceps skinfold measurements half those of white Canadians and Americans. Serum cholesterol levels were also low, and markers for diabetes, hypertension, and cardiovascular disease were missing among them (Eaton, Konner, and Shostak 1988; Raichlen et al. 2016).
Health Consequences of the Transition to Agriculture and Animal Domestication
The shift from foraging to food production occurred relatively recently in our evolutionary history (Larsen 2014), and there are indications our biology has not yet caught up (Pritchard 2010). Beginning around 12,000 BCE in several parts of the globe, humans began to move toward a diet based on domesticated plants and animals (Armelagos et al. 2005). This involved manipulating the natural landscape to facilitate intensive food production, including the clearing of forest and construction of wells, irrigation canals, and ditches, exposing humans to water-borne illnesses and parasites and attracting mosquitos and other vectors of disease to human settlements. The heavy, repetitive physical labor of early agricultural production resulted in negative impacts on articular joints, including osteoarthritis (Larsen 2014). At the same time, nutritional diversity became restricted, focused on major cereal crops that continue to dominate agricultural production today, including corn, wheat, and rice (Jain 2012). This represented a major shift in diet from a wide variety of plant and animal foods to dependence on starchy carbohydrates, leading to increases in dental caries (cavities), reductions in stature and growth rates, and nutritional deficiencies (Larsen 2014). Domesticated animals added new foods to the human diet, including meat that was higher in fat and cholesterol than wild game as well as dairy products (Lucock et al. 2014). Agriculture provided the means to produce a storable surplus for the first time in human history, leading to the beginnings of economic inequality (see Chapter 12). Social hierarchies led to the unequal distribution of resources, concentrating infectious disease among the poor and malnourished (Zuckerman et al. 2014), a situation that continues to plague humanity today (Marmot 2005).
Sedentism and a rise in population density accompanied the move to agriculture, increasing the risk of infectious disease. Agriculture often provided enough calories, if not enough nutrition, to increase fertility. Although diets were worse and people unhealthier, populations continued to grow, even in the midst of high levels of child and maternal mortality and short life expectancies (Omran 2005). Hygiene became an issue as large settlements increased the problem of removing human waste and providing uncontaminated water (Armelagos et al. 2005). Domesticated animals provided reservoirs of zoonotic pathogens, which affected farmers more than foragers, as farmers were in closer proximity to their animals on a daily basis (Marciniak and Perry 2017). Many of these diseases became major killers of humankind, including influenza, tuberculosis, malaria, plague, syphilis, and smallpox, functioning as selective pressures in and of themselves (Cooling 2015). As these diseases encountered large human populations, they caused major epidemics that traveled along newly established routes for trade, warfare, and colonization.
Epidemiological Transitions
Changes in diet and physical-activity patterns, population densities, and exposure to zoonoses associated with agriculture resulted in an epidemiological transition, a shift in the causes of morbidity (sickness) and mortality (death) among humankind (Omran 2005). The first epidemiological transition from foraging to food production resulted in increases in dental caries (see Chapter 12), nutritional deficiencies, infectious disease, and skeletal conditions like osteoarthritis, as well as decreases in growth and height (Larsen 2014). A second epidemiological transition occurred following the Industrial Revolution in Western Europe and the United States when improved standards of living, hygiene, and nutrition minimized the effects of infectious disease, after which people began to experience higher rates of noncommunicable diseases, such as cancer, heart disease, and diabetes due to the changes in lifestyle, diet, and activity levels that are the subject of this chapter (Omran 2005). With the addition of immunizations and other public health initiatives, modified forms of this transition remain ongoing in many low- and middle-income countries (Zuckerman et al. 2014), with several now facing a “double burden” of disease, with poor, often rural, populations struggling with infectious diseases due to malnutrition, lack of sanitation, and access to health care, while more affluent citizens are victims of chronic illnesses. A third epidemiological transition is now underway as infectious diseases, including new, re-emergent, and multidrug-resistant diseases, have once again become major health concerns (Harper and Armelagos 2010; Zuckerman et al. 2014). These include COVID-19, Ebola, HIV/AIDS, tuberculosis, malaria, dengue, Lyme disease, and West Nile virus—all zoonoses that initially spread to humans through contact with animals.
Patterns of morbidity and mortality continue to shift across the globe. As with the first epidemiological transition resulting from the adoption of large-scale agriculture, such shifts can be the direct, if unintended, result of human interactions with the environment. For example, there has been a rise in chronic inflammatory diseases (CIDs) in developed countries (Versini et al. 2015). This includes increased rates of allergic conditions like asthma and autoimmune diseases like rheumatoid arthritis, multiple sclerosis, Crohn’s disease, and inflammatory bowel disease. This has coincided with the decrease in infectious disease associated with the second epidemiological transition, and the two are related. The “hygiene hypothesis” postulates the rise in CIDs is a result of limited exposure to nonlethal environmental pathogens in utero and early childhood (Zuckerman and Armelagos 2014). Modern human societies have become so sanitized that we are no longer exposed to microorganisms that stimulate the development of a healthy immune system (Versini et al. 2015). “In effect, the lifestyle changes—sanitary improvements, pasteurization, use of antibiotics, and improved hygiene—that contributed to the second transition may have produced a substantial trade-off, with developed nations exchanging a high burden of infectious disease for a higher burden of CIDs” (Zuckerman et al. 2014).
The third epidemiological transition, the re-emergence of infectious disease, reflects the continuing relationship between humans, animals, and pathogens. Over 60% of emerging infectious diseases (EIDs) since 1940 have been of zoonotic origin, with over 70% stemming from human contact with wildlife (Jones et al. 2008), including COVID-19. The crossover of COVID to humans is believed to have involved transmission from bats to an intermediate species then to humans, with infected humans then passing it to other humans in a wet market in Wuhan, China in late 2019 (Worobey et al. 2022). Two COVID variants, representing two distinct crossover events from animals to humans, were circulating in the market by February 2020. Similarly, the global bushmeat trade currently devastating Africa’s wildlife is a continuing source of Ebola infection (Asher 2017), as well as the original source of HIV and viruses related to leukemia and lymphoma among humans (Zuckerman et al. 2014). New strains of avian (bird) flu, some with mortality rates as high as 60% among humans (WHO n.d.), are transmitted to humans through poultry production and contact with wild birds (Davis 2005). Lastly, the use of antibiotics in commercial meat production is directly related to the rise of drug-resistant strains of previously controlled infectious diseases. An estimated 80% of antibiotics in the U.S. are used to promote growth and prevent infection in livestock, and drug-resistant bacteria from these animals are transmitted to humans through meat consumption (Ventola 2015).

A fourth epidemiological transition is currently underway in which some parts of the globe are suffering from a “triple burden” of infectious and chronic diseases combined with injuries and diseases related to intensifying globalization, urbanization, deforestation, and climate change (Karn and Sharma 2021). Massive flooding in Pakistan in 2022 (Figure 16.3) will serve to illustrate the concept. Following a severe heat wave in June 2022, Pakistan experienced extremely heavy seasonal monsoon rains, in some provinces 700% above normal. Combined with water flow from melting glaciers, this caused the worst flooding in the country’s history, putting one third of the nation under water (Sheerazi 2022). The heat wave, glacial melt, and extreme rainfall were all attributable to global climate change, inflicting destruction and disease on Pakistan, which produces less than 1% of total global carbon emissions (Government of Pakistan 2021).
As a direct result of the flooding, infrastructure, including roads, homes, and bridges, was destroyed, and 1,700 people died, nearly 13,000 were injured, and over 33 million were displaced. In addition to their initial injuries and trauma, displaced people lacked food, health care, safe water, and basic sanitation, leading to starvation and exposure to infectious diseases like malaria and dengue fever, as well as skin conditions like scabies, caused by mites. Pakistan also has a poverty rate of 30–40%, contributing to already-high rates of HIV, tuberculosis, and hepatitis. At the same time, the leading causes of death are heart disease, cancer, lower respiratory diseases, and stroke (CDC n.d), all chronic conditions.
These examples illustrate continuing interaction between humans, our evolved biology, and the physical and cultural environments in which we live. The remainder of this chapter will focus on selected diseases and the social, cultural, and environmental factors that contribute to their prevalence in modern, industrialized economies. We begin with the health condition that affects all of the others—obesity.
Obesity
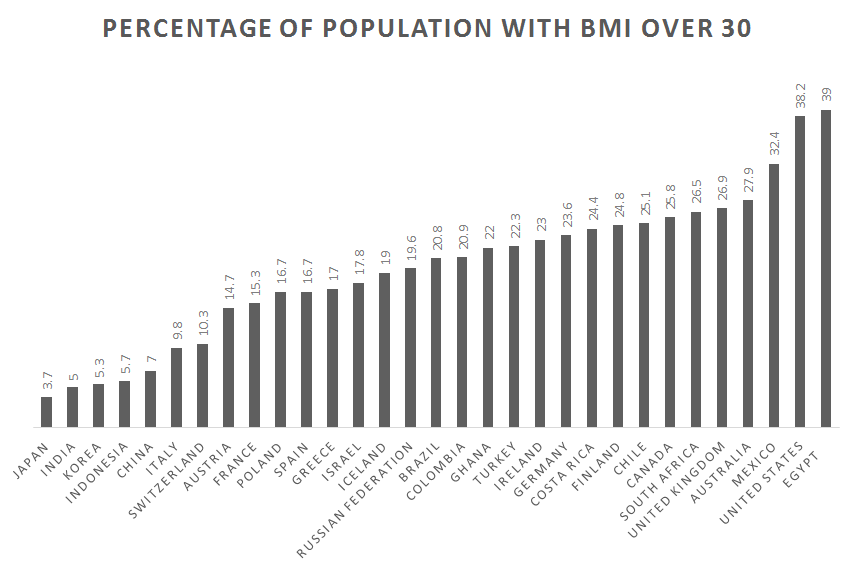
According to the World Health Organization (2017), 1.9 billion of the world’s people are overweight and 650 million of these are obese. In the United States, 70% of Americans are overweight, and 40% of these meet the criteria for obesity. For the first time in human history, most of the world’s population lives in countries where overweight and obesity kill more people than hunger (Figure 16.4). Improvements in public health and food production have allowed a greater number of people to live past childhood and to have enough to eat. This does not include everyone. Many people still struggle with poverty, hunger, and disease, even in the wealthiest of nations, including the United States. On a global scale, however, many people not only have enough food to survive but also to gain weight—enough extra weight to cause health problems.
Although studies show differences in daily energy expenditure between foraging and farming populations compared with industrialized peoples, the major contributor to obesity in Western populations is energy intake (Pontzer et al. 2012). Many people not only eat too much but too much of the wrong things. Biological anthropologist Leslie Lieberman (2006) argues that contemporary humans continue to rely on cues from foraging strategies of our evolutionary past that are now counterproductive in the obesogenic environments in which we now live.
Examine your own eating habits in the context of how humans once hunted and gathered. Humans once relied on visual cues to find food, often traveled long distances to obtain it, then transported it back to our home base. There they may have had to process it by hand to render it edible. Think of how much less energy it takes to find food now. If we have the financial resources, we can acquire big energy payoffs by simply sitting at home and using an app on our mobile phone to place an order for delivery. And, voila! High-calorie (if not highly nutritious) food arrives at our door. Should we venture out for food, search time is reduced by signage and advertising directing us toward high-density “patches” where food is available 24 hours a day. These include vending machines, gas stations, and fast-food outlets. Travel time is minimal and little human energy is used in the process (Lieberman 2006).
Foods are also prepackaged and prepared in ways that allow us to eat large quantities quickly. Think French fries or chicken nuggets, which we can easily eat with our hands while doing other things, like driving or watching television, rendering eating mindless and allowing us to take in food faster than our endocrine systems can tell us we are getting full. Modern “patches” offer low-fiber, calorie-dense resources, which allow us to eat larger quantities, a problem already encouraged by larger portion sizes (Lieberman 2006). Processed foods are also engineered to appeal to human preferences for sweet tastes and fatty, creamy textures (Moss 2013). Remember from earlier chapters that natural selection favored depth perception, color vision, grasping hands, and coordinated eye-hand movements as general primate traits. Advertising and packaging now use our color vision against us, attracting us to products that have little nutritional value but that play to our evolutionary predisposition toward variety. Remember those 50 different nutrients we require? That variety is now presented to us in the form of 55 different flavors of Oreo cookies (Cerón 2017), which we take out of the package and dip in milk using our hand-eye coordination and depth perception.
Even if we are ostensibly eating the same things our ancestors did, these foods are nothing alike. Take potatoes, for example. One medium-sized, plain, baked potato is a healthy food, especially if we eat the skin too. It contains 110 calories, 0 grams of fat, 26 grams of carbohydrates, and 3 grams of protein, plus 30% of the U.S. Recommended Daily Allowance (RDA) of vitamin C, 10% of vitamin B6, 15% of potassium, and no sodium (Potato USA). In contrast, a medium order of McDonald’s fries, which takes the potato and adds salt and fat, contains 340 calories, 16 grams of fat, 44 grams of carbohydrates, 4 grams of protein, and 230 mg of sodium (McDonalds). Potato chips take food processing to a whole new level, removing even more nutrition and adding a host of additional ingredients, including oils, preservatives, and artificial flavorings and colors (Moss 2013). Take Ruffles Loaded Bacon and Cheddar Potato Skins Potato Chips as an example (St. Pierre 2018). The number of ingredients increases from one to 11 to 35 as we move from the potato to the potato chip, moving further from nature with each step (Figure 16.5). It should be noted that the nutritional information for the potato chips is based on a serving size of 11 chips, an amount likely smaller than many people eat. Many sweet, fatty, salty foods like fries and chips are cheap, which is why many people choose to eat them (Moss 2013). The price of a medium-sized order of McDonald’s fries as of this writing is US$1.79, and the potato chips are $2.98 for an 8.5-ounce bag. A single potato prewrapped for microwaving is available in many supermarkets for US$1.99 but requires access to a microwave and eating utensils, making it less convenient.
|
|

French Fries |
|
|
|---|---|---|---|
| Calories | 110 | 340 | 160 |
| Calories from fat | 0 | 144 | 90 |
| Fat | 0g | 16g | 10g |
| Carbohydrates | 26g | 44g | 15g |
| Protein | 3g | 4g | 2g |
| Sodium | 0g | 230mg | 170mg |
| Dietary fiber | 2g | 4g | 1g |
| Sugars | 1g | 0g | 1g |
| Cholesterol | 0g | 0g | 0g |
| Ingredients | Potato | Potatoes, vegetable oil (canola oil), soybean oil, hydrogenated soybean oil, natural beef flavor (wheat and milk derivatives), citric acid (preservative), dextrose, sodium acid pyrophosphate (main color), salt. | Potatoes, vegetable oil (sunflower, corn, and/or canola oil), bacon and chedder loaded potato skins seasoning (maltodextrin – made from corn) salt, cheddar cheese (milk, cheese cultures, salt enzymes), sour cream (cultured cream, skin milk), whey, dried onion, monosodium. |
Not only have we transformed the food supply and our eating in ways that are detrimental to our health, but these changes have been accompanied by reductions in physical activity. Sedentarism is built into contemporary lifestyles. Think of how much time you spent sitting down today. Some of it may have been in class or at work, some may have been driving a car or perhaps binge-watching your favorite show, playing a video game, or checking in on social media. An inactive lifestyle is almost dictated by the digital age (Lucock et al. 2014). Levels of physical activity in many countries are now so low that large portions of the population are completely sedentary, including one in five Americans (CDC 2022). For a species whose biology evolved in an environment where walking, lifting, and carrying were part of daily life, this is unhealthy and often leads to weight gain.
Biology and Genetics of Weight
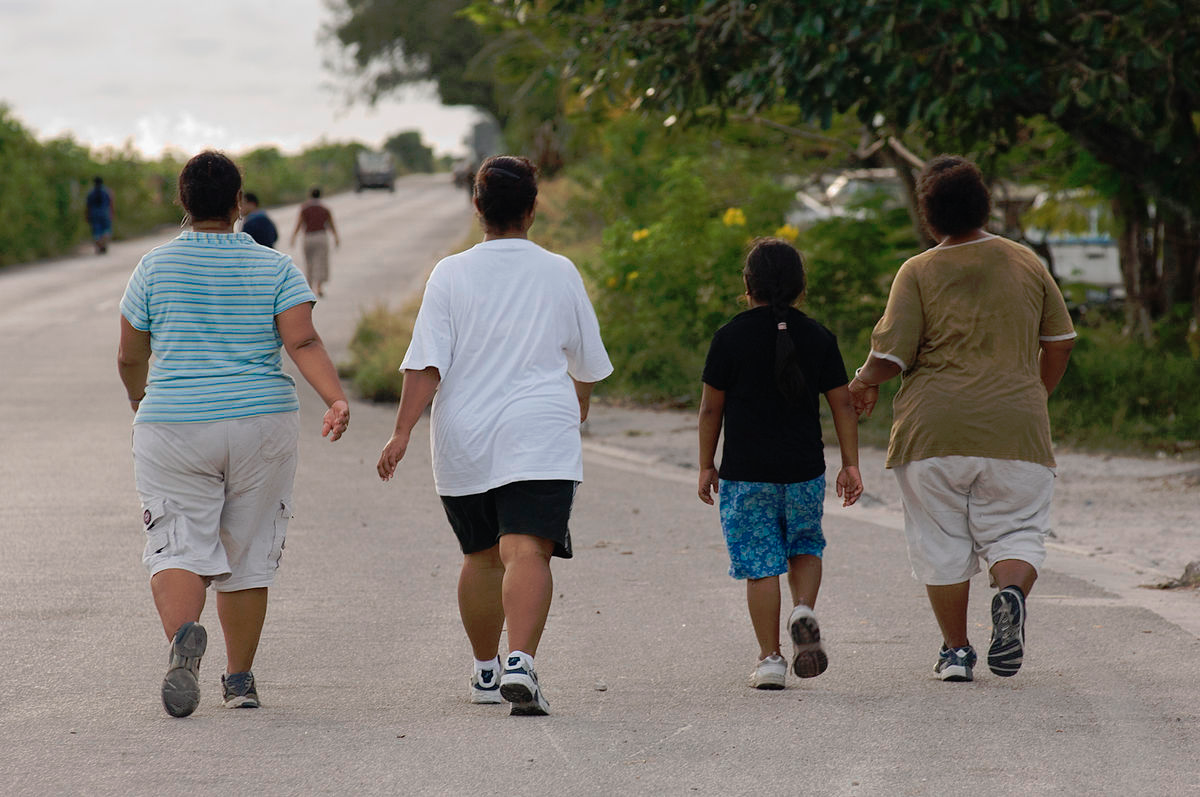
Research indicates multiple genetic variants influence weight gain, and they are not spread evenly among human populations. Tuomo Rankinen and colleagues (2006) identified 127 genes associated with obesity, of which 22 contributed to weight gain. Claude Bouchard (2007) then identified five categories of obesity-promoting genotypes. These genotypes promote sedentarism, result in low metabolism, and lead to poor regulation of appetite, and a propensity to overeat. An example of the impact such genotypes can have in an environment of plenty is found among the population of the Micronesian island of Nauru. Historically, the island was geographically isolated and the food supply was unpredictable. These conditions favored genotypes that promoted the ability to rapidly build up and store fat in times of food availability. In Nauruans, there are two genetic variants favoring weight gain and insulin resistance, and both are associated with obesity and type 2 diabetes. One variant is also associated with hypertension. One of these variants is also found in Pima Indians, who live in parts of Arizona and Mexico. In the Pima, this variant is associated with a high body mass index (BMI) and type 2 diabetes, although it is not associated with the same outcomes in Japanese and British subjects (de Silva et al. 1999). The other variant was analyzed in Finnish and South Indian populations, neither of whom experienced the same outcome as Nauruans. This suggests these alleles may act as modifying genes for type 2 diabetes in some population groups (Baker et al. 1994). Unfortunately, Nauruans are one of those groups. Eventually, they became wealthy through phosphate mining on the island, gaining access to a calorie-rich Western diet of imported foods and developing a sedentary lifestyle. This resulted in rates of type 2 diabetes as high as 30–40% in Nauruans over the age of 15, which became the leading cause of death (Lucock et al. 2014), something Nauruans are taking seriously (Figure 16.6).
Factors other than biology influence which populations that carry a genetic predisposition to diabetes actually express it. The Pima Indians of Arizona, for example, were seriously impacted by U.S. government policies that affected water rights, forcing the population away from subsistence farming to dependence on government handouts and convenience food. This resulted in a significant loss of physical activity, malnutrition, and obesity. The Pima continue to experience hardship due to high rates of unemployment, poverty, and depression, sometimes made worse by alcoholism. In the absence of these pressures, the Pima were diabetes free for centuries prior, even though they relied on agriculture for subsistence, suggesting genetics alone is not responsible for high rates of obesity and diabetes in current Pima Indian populations (Smith-Morris 2004).
Obesity also has an epigenetic component. You learned about epigenetics in Chapter 3. With regard to obesity, epigenetics is counterintuitive in that mothers who do not take in enough calories during pregnancy often give birth to babies who grow up to be fat. What takes place is the fetus receives signals during pregnancy from its mother through the placenta and intrauterine environment about environmental conditions outside of the womb, in this case food insecurity. These signals encourage the turning on and off of genes related to metabolism. This alters the phenotype of the fetus so that if the child is born into an environment where food is plentiful, it will put on weight rapidly whenever possible, leading to obesity and related diseases later in life. If the child is a girl, her own eggs are formed in utero with the same genetic changes coded in, meaning she will pass along this same genetic predisposition to gain weight to her children. Hence, a biological propensity toward obesity can continue across generations (Worthman and Kuzara 2005). Epigenetic changes to genes that promote weight gain are argued to be partly responsible for the rapid rise in obesity and diabetes in developing countries gaining access to Western diets (Stearns, Nesse, and Haig 2008).
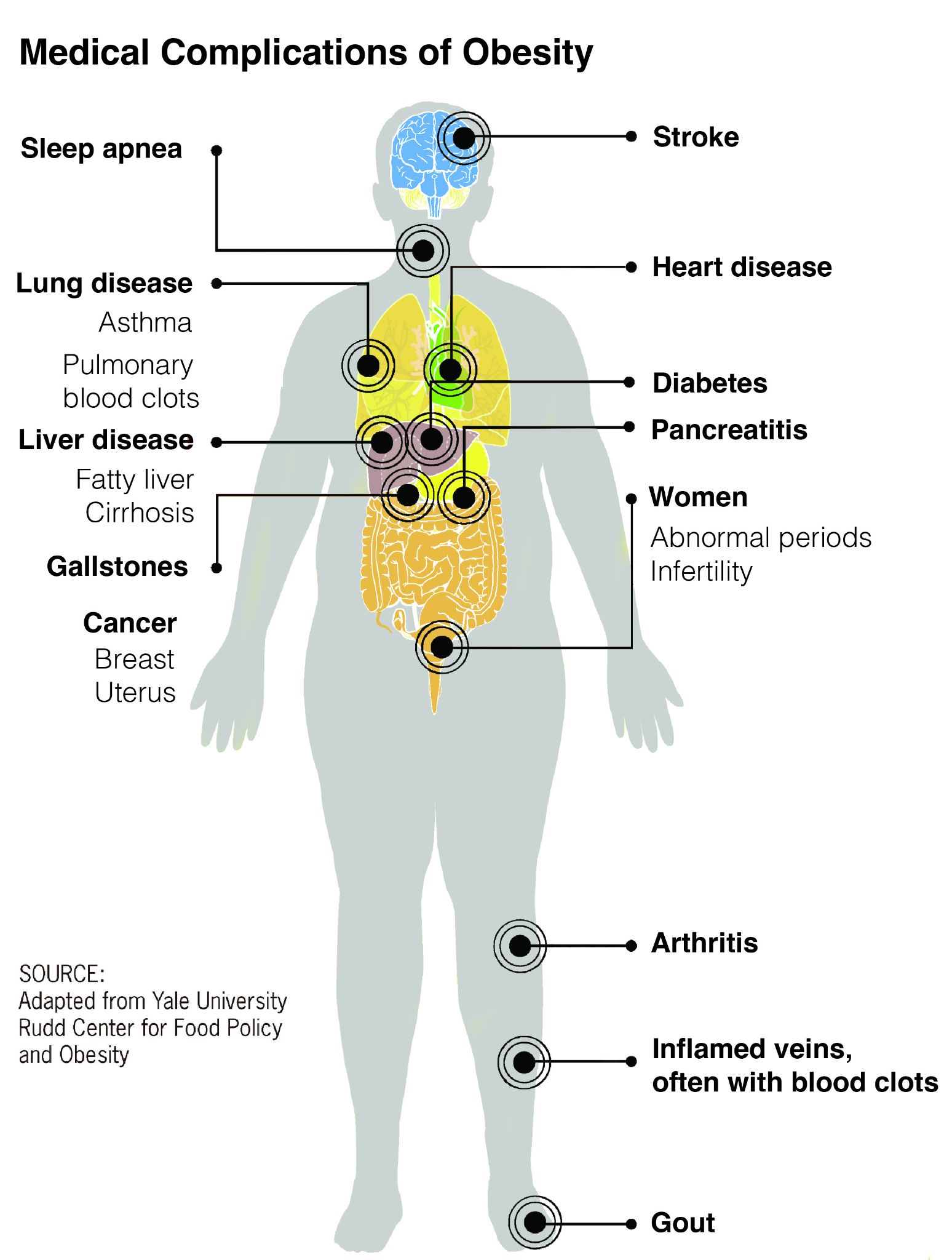
Obesity and overweight put a strain on several biological systems of the body, including the circulatory, endocrine, and skeletal systems, contributing to hypertension, heart disease, stroke, diabetes, and osteoarthritis (Figure 16.7). Obesity also elevates the risk of cancers of the breast, endometrium, kidney, colon, esophagus, stomach, pancreas, and gallbladder (National Institutes of Health 2017; Vucenik and Stains 2012). Diabetes—one of the fastest-growing health conditions around the globe (WHO 2016) and one tightly connected to obesity and overweight—is the focus of the following Special Topics box.
Special Topic: Diabetes
Diabetes mellitus is an endocrine disorder characterized by excessively high blood glucose levels (Martini et al. 2013). According to a report released by the World Health Organization, the number of people living with diabetes is growing in all regions of the world. Rates of diabetes have nearly doubled in the past three decades, largely due to increases in obesity and sugary diets (WHO 2016). One in 10 people around the world, 537 million people, now have diabetes, and three out of four live in low- and middle-income countries (IDF 2022). In the United States, 37 million people have diabetes (CDC 2020), where the disease is rising fastest among millennials (those ages 20–40) (BCBSA 2017), and one in every two adults with diabetes is undiagnosed (IDF 2022). Obesity and diabetes are linked: obesity causes a diet-related disease (diabetes) because of humans’ evolved metabolic homeostasis mechanism, which is poorly suited to contemporary energy environments (Lucock et al. 2014).
To function properly, cells need a steady fuel supply. Blood sugar (glucose) is the fuel for most cells in the body, and the body produces the hormone insulin to help move glucose into cells that need it (Figure 16.8). Foods that most readily supply glucose to your bloodstream are carbohydrates, especially starchy foods like potatoes or sweet, sugary foods like candy and soda. The body can also convert other types of foods, including protein-rich foods (e.g., lean meats) and fatty foods (e.g., vegetable oils and butter), into blood sugar in the liver via gluconeogenesis. Insulin’s main job is to tell your cells when to take up glucose. The cell also has to listen to the signal and mobilize the glucose transporters. This not only allows your cells to get the energy they need, but it also keeps blood sugar from building up to dangerously high levels when you are at rest.
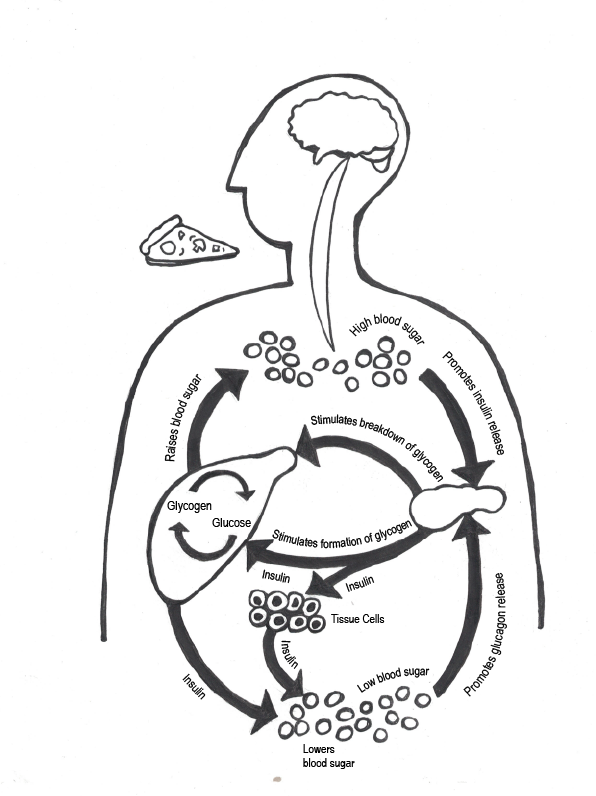
This system has limits. Like the rest of our biology, it evolved during several million years when sugar was hard to come by and carbohydrates took the form of fresh foods with a low glycemic index (GI). Our ancestors were also active throughout the day, taking pressure off of the endocrine system. Now, sedentary lifestyles and processed-food diets cause many of us to take in more calories—and especially more carbohydrates—than our bodies can handle. There is only so much blood sugar your cells can absorb. Many modern populations are taxing those limits. After years of being asked by insulin to take in more glucose than they can use, cells eventually stop responding (McKee and McKee 2015). This is called type 2 diabetes or insulin resistance, which accounts for 90–95% of diabetes cases in the United States (Figure 16.9). type 1 diabetes is believed to be caused by an autoimmune response in which your immune system is attacking and destroying the insulin-producing cells in your pancreas (Figure 16.9). type 1 diabetes is a genetic condition that often shows up early in life, while type 2 is more lifestyle-related and develops over time.
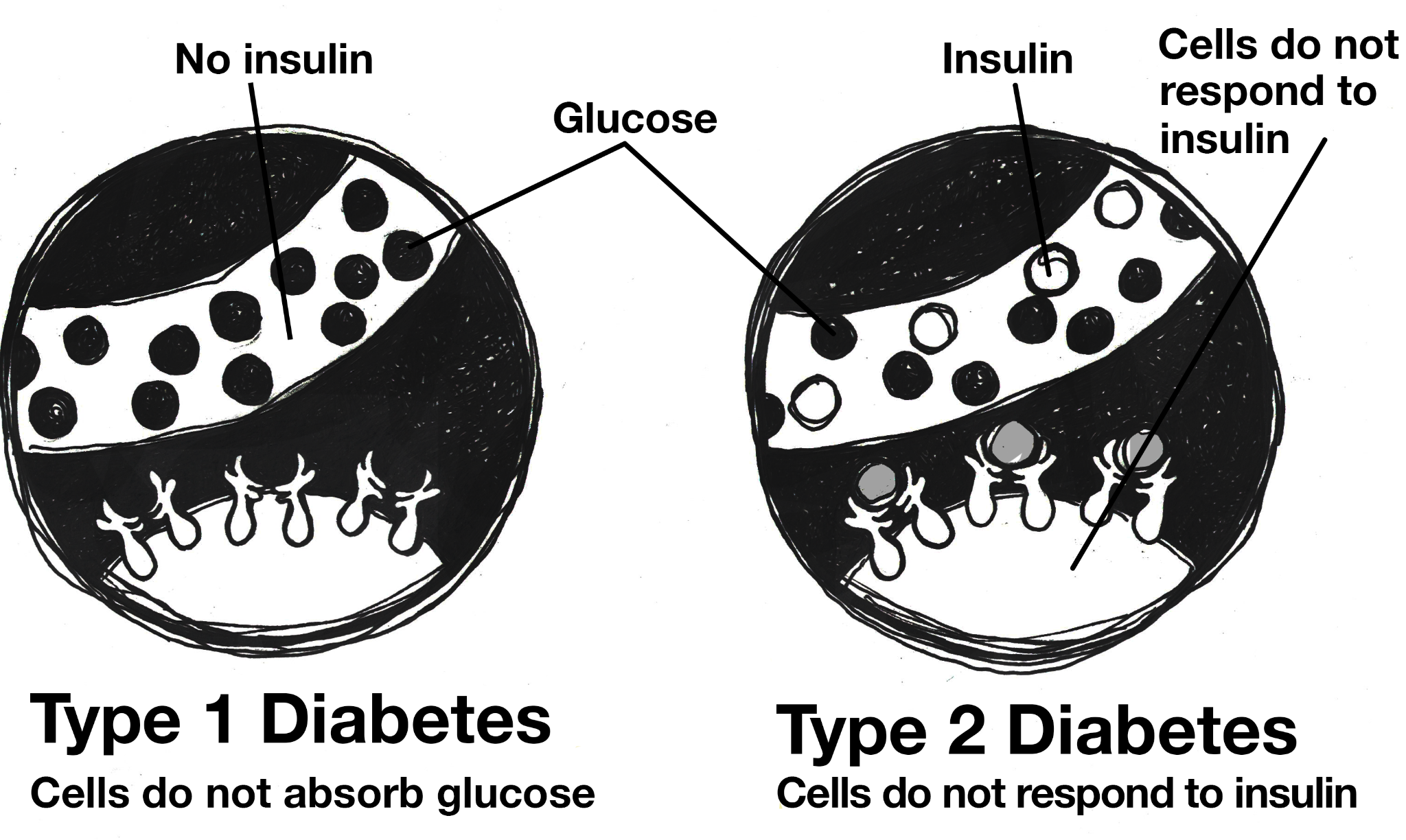
Cardiovascular Disease
Cardiovascular disease (CVD)—which includes coronary heart disease, hypertension (high blood pressure), and stroke—is the leading cause of death globally, and heart disease remains the number one cause of death in the United States (American Heart Association 2018). Risk factors for cardiovascular disease include diet, obesity/overweight, diabetes, smoking and alcohol consumption, and physical inactivity.
The connections between these factors and heart disease may not seem obvious and will be addressed here beginning with diet. Diets high in saturated fat and cholesterol can lead to atherosclerosis, a condition in which fat and cholesterol form plaque inside the arteries, eventually building up and hardening to the point that blood flow is blocked. Too much salt in the diet leads to fluid retention, which increases blood volume and thereby blood pressure, taxing the heart. Obesity/overweight contribute to cardiovascular disease directly through increases in total blood volume, cardiac output, and cardiac workload. In other words, the heart has to work much harder if one is overweight (Akil and Ahmad 2011). Obesity also relates to CVD indirectly through elevation of blood pressure (hypertension) and diabetes. High levels of blood glucose from diabetes can damage blood vessels and the nerves that control the heart and blood vessels. Alcohol consumption can raise blood pressure and triglyceride levels, a type of fat found in the blood. Alcohol also adds extra calories, which may cause weight gain, especially around the abdomen, which is directly associated with risk of a heart attack (Akil and Ahmad 2011). Cigarette smoking also increases the risk of coronary heart disease. Nicotine increases blood pressure; in addition, cigarette smoke causes fatty buildup in the main artery in the neck and thickens blood, making it more likely to clot. It also decreases levels of HDL (“good”) cholesterol (American Heart Association 2018). Even secondhand smoke can have an adverse effect if exposure occurs on a regular basis. Chronic psychological stress also elevates the risk of heart disease (Dimsdale 2008). The repeated release of stress hormones like adrenaline elevates blood pressure and may eventually damage artery walls. The human stress response and its connections to health and disease are discussed in more detail below.
However, physical activity alters the likelihood of having heart disease, both directly and indirectly. Regular exercise of moderate to vigorous intensity strengthens the heart muscle and allows capillaries, tiny blood vessels in your body, to widen, improving blood flow. Regular exercise can also lower blood pressure and cholesterol levels and manage blood sugar levels, all of which reduce the risk of CVD.
Cancer
Cancer is the second-leading cause of death globally, causing one in every six deaths and killing nearly nine million people in 2015 (WHO 2018). Lifetime cancer risk in developed Western populations is now one in two, or 50% (Greaves 2015). Approximately one-third of deaths from cancer are due to behavioral and dietary factors, including high body mass index (BMI), low fruit and vegetable intake, lack of physical activity, and the use of tobacco and alcohol. Depending on the type of cancer and one’s own genetic inheritance, these factors can increase cancer risk from 2- to 100-fold (Greaves 2015). Cancer is the result of interactions between a person’s genes and three categories of external agents: physical carcinogens (e.g., ultraviolet radiation), chemical carcinogens (e.g., tobacco smoke, asbestos), and biological carcinogens, such as infections from certain viruses, bacteria, or parasites (WHO 2018). Obesity is also a risk factor for cancer, including of the breast, endometrium, kidney, colon, esophagus, stomach, pancreas, and gallbladder (National Institutes of Health 2017; Vucenik and Stains 2012).
Cancer has been regarded as a relatively recent affliction for humans that became a problem after we were exposed to modern carcinogens and lived long enough to express the disease (David and Zimmerman 2010). Given the long history that humans share with many oncogenic (cancer-causing) parasites and viruses (Ewald 2018), and the recent discovery of cancer in the metatarsal bone of a 1.8-million-year-old hominin (Odes et al. 2016), this view is being challenged (See “Special Topic: Life Choices and Reproductive Cancers in Women”). The difficulties of identifying cancer in archaeological populations are many. Most cancer occurs in soft tissue, which rarely preserves, and fast-growing cancers would likely kill victims before leaving evidence in bone. It is also difficult to distinguish cancer from benign growths and inflammatory disease in ancient fossils, and there is often postmortem damage to fossil evidence from scavenging and erosion. However, using 3-D images, South African researchers recently diagnosed a type of cancer called osteosarcoma in a toe bone belonging to a human relative who died in Swartkrans Cave between 1.6 and 1.8 million years ago (Randolph-Quinney et al. 2016). This study provides the earliest evidence of cancer in hominins.
Special Topic: Life Choices and Reproductive Cancers in Women
Behavioral or “lifestyle” choices have an impact on cancer risk. Breast cancer is one example. It is the most common cancer in women worldwide, but incidence of new cases varies from 19.3 per 100,000 women in Eastern Africa to 89.7 per 100,000 women in Western Europe (WHO 2018). These differences are attributable to cultural changes among women in Western, industrialized countries that are a mismatch for our evolved reproductive biology. Age at menarche, the onset of menstrual periods, has dropped over the course of the last century from 16 to 12 years of age in the U.S. and Europe, with some girls getting their periods and developing breasts as young as eight years old (Greenspan and Deardorff 2014, Figure 16.10). A World Health Organization study involving 34 countries in Europe and North America suggests the primary reason for the increase in earlier puberty is obesity, with differences in BMI accounting for 40% of individual- and country-level variance (Currie et al. 2012). Early puberty in girls is associated with increased risk of breast cancer, ovarian cancer, diabetes, and high cholesterol in later life (Pierce and Hardy 2012).
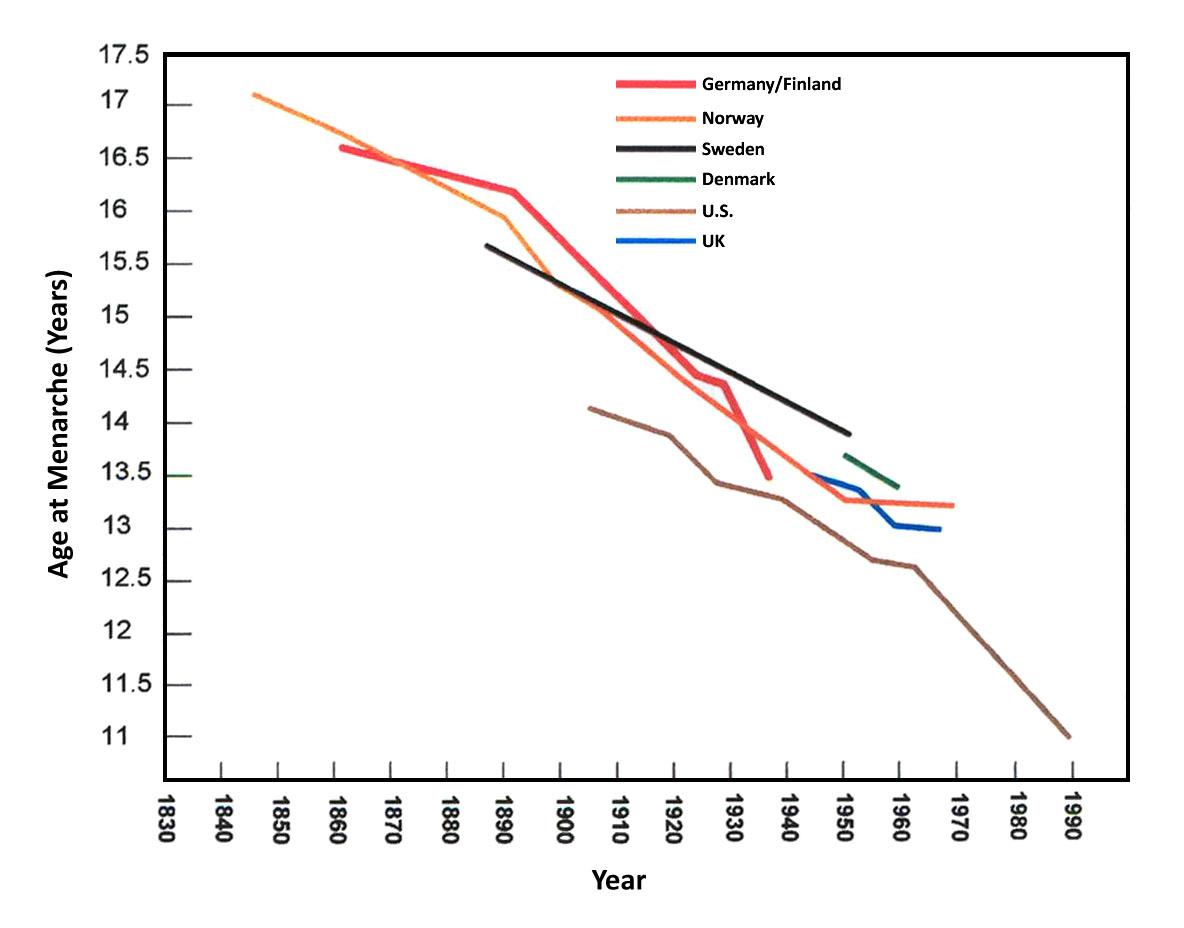
At the same time that age at puberty is dropping for girls in Western nations, age at birth of the first child is later, at 26 years old (Mathews and Hamilton 2016). Women are also having fewer children, two on average (Gao 2015), with 15% of women choosing to remain childless (Livingston 2015). Rates of breastfeeding have risen in recent decades but drop to only 27% of infants once babies reach 12 months of age (CDC 2014). In contrast, data from modern foraging populations (Eaton et al. 1994) indicate that age at menarche is around 16 years old, age at birth of the first child is 19, breastfeeding on-demand continues for three years for each child, and the number of children averages six. These differences relate to elevated risk for reproductive cancers, including breast cancer, among women in developed countries.
Other than an established genetic risk (e.g., BRCA gene), the primary risk factor for breast cancer is exposure to estrogen. For women living in modern, industrialized economies, this exposure now often comes from women’s own ovaries rather than from external environmental sources (Stearns, Nesse, and Haig 2008). There is nothing biologically normal about regular monthly periods. Women in cultures without contraception are pregnant or breastfeeding for much of their reproductive lives, resulting in 100 or so menstrual cycles per lifetime. In contrast, Western women typically experience 400 or more (Strassmann 1997). This is partly due to early puberty. From menarche to the birth of a woman’s first child can be 14 years or longer in Western populations, after which breastfeeding, if undertaken at all, lasts for a few weeks or months. Oral contraceptives or other hormonal methods to control reproduction induce monthly periods. Age at menopause (the cessation of menstrual cycles) is 50–55 years old across human populations. For Western women, this translates into forty years of menstrual cycling. Each month the body prepares for a pregnancy that never occurs, experiencing cell divisions that put women at risk for cancers of the breast, endometrium, ovaries, and uterus (Strassmann 1999). Obesity adds to risk, as adipose (fat) tissues are the main source of estrogen biosynthesis. Thus, weight gain during the postmenopausal stage means higher exposure to estrogen and a greater risk of cancer (Ali 2014).
Women cannot return to our evolutionary past, and there are important social and economic reasons for delaying pregnancy and having fewer children. These include achieving educational and career goals, greater earning power, a reduction in the gender pay gap, more enduring marriages, and a decrease in the number of women needing public assistance (Sonfield et al. 2013). There are also cultural means by which we might reduce the risk of reproductive cancers. These include reformulating hormonal contraceptives with enough estrogen to maintain bone density but reducing the number of menstrual periods over the reproductive lifespan (Stearns, Nesse, and Haig 2008). Reducing fat intake may also lower estrogen levels. High-fat diets contribute to breast tumor development, while high fiber diets are beneficial in decreasing intestinal resorption of estrogenic hormones. Exercise also appears protective. Studies of former college athletes demonstrate risks of breast, uterine, and ovarian cancers later in life two to five times lower than those of nonathletes (Eaton et al. 1994).
Stress
Have you ever been “stressed out” in class? Say you’re in a large lecture hall with a hundred other people, or even in a small class where you don’t know anyone. You’re not sure about something the professor just said and you would really like to ask about it, so you start to raise your hand. Does your heart begin to pound and your mouth become dry? Do you get so nervous that you choose to ask a classmate after lecture instead? If so, you are not alone. Fear of speaking in public is one of the most common social phobias (APA 2013). It has been estimated that 75% of all people experience some degree of anxiety or nervousness when it comes to public speaking (Hamilton 2011), and surveys have shown that most people fear public speaking more than they fear death (Croston 2012).
We have evolution to thank for this.
Humans, like other primates, are social animals. Being part of a group helped us to survive predation, get enough to eat, and successfully raise our young. When faced with standing up in front of a group, or even speaking up in class, we break into a sweat because we are afraid of rejection. Psychologist Glenn Croston (2012) writes, “The fear is so great because we are not merely afraid of being embarrassed or judged. We are afraid of being rejected from the social group, ostracized and left to defend ourselves all on our own. We fear ostracism still so much today it seems, fearing it more than death, because not so long ago getting kicked out of the group probably really was a death sentence.” Hence, it is no surprise that public speaking triggers a stress response among much of humankind.
The human nervous system evolved in a context where quick responses to perceived threats presented an evolutionary advantage. The “fight or flight” response was honed during millions of years when threats more often took the form of an approaching lion than an approaching deadline. Our body’s stress response, however, is triggered by a wide variety of stressors that produce the same general pattern of hormonal and physiological adjustments (Martini et al. 2013). In today’s world, the system is often stuck in the “on” position due to the constant pressures of modern life, and this is a significant influence on health and disease.
It is important to recognize that there are different types of stress and the time in life when adult coping mechanisms are formed is in childhood. In children, some stressors can be positive—for example, stressors that are mild to moderate in magnitude, and accompanied by the support of a caring adult, which help children develop pathways by which stress is dealt with by the body throughout life. In a young child, a positive stress response might be going to the pediatrician to receive a vaccination and receiving encouragement and comfort from both parent and practitioner. A tolerable stress response is more serious, precipitated by something like a divorce or death of a relative. Again, buffered by positive support from surrounding adults, these types of stressors can be successfully managed by children. Toxic stress, however, “results from strong, frequent or prolonged activation of the stress response in the absence of the buffering protection of a supportive adult relationship” (Shonkoff and Garner 2012). Examples include child abuse or neglect, parental substance abuse, homelessness, and violence. In the absence of adequate psychological and physical support, the biological pathways of a child’s physiological stress response are altered and lead to reduced abilities to cope with life’s challenges as an adult.
The negative effects of sustained, elevated cortisol levels on health are well documented. These include higher levels of infectious disease and slowed growth in childhood (Flinn and England 2003) and increased incidence of heart disease, obesity, and diabetes in adults (Worthman and Kuzara 2005). Contrary to our evolutionary past, many causes of sustained stress in contemporary societies are psychosocial rather than physical threats. These can include an unhappy marriage or frustrations at work (Dimsdale 2008). Stressors can also be more subtle. For example, a review of research into the effects of stress on health indicated that experiencing racism was a significant stressor that was associated with alcohol consumption, psychological distress, overweight, abdominal obesity, and higher fasting-glucose levels among minority groups (Williams and Mohammed 2013). Chronic, everyday racial discrimination is also associated with the hardening of coronary arteries, elevated blood pressure, giving birth to lower-birth-weight infants, cognitive impairment, poor sleep, and visceral fat, which is fat stored deep inside the belly, wrapped around the organs, including the liver and intestines. Visceral fat is a sign of metabolic syndrome, increasing the risk of stroke, heart disease, and type 2 diabetes. These effects have been shown to increase morbidity and mortality among members of affected groups.
Epigenetics can also be a factor in how a person is able to deal with stressful situations. Maternal experiences of stress during pregnancy have the potential to permanently alter the physiology of mothers’ offspring, especially the hypothalamic-pituitary-adrenal (HPA) axis. The HPA axis regulates metabolism, blood pressure, and the immune response, and these alterations can predispose prenatally stressed individuals to suffer metabolic, cardiovascular, and mental disorders in adulthood (Palma-Gudiel et al. 2015). These experiences carry across generations, with children of Holocaust survivors who experienced PTSD demonstrating similar changes in neurochemistry in the absence of a sustained, traumatic event, as did infant offspring of mothers who developed PTSD during pregnancy after witnessing the traumatic events of 9/11 (Yehuda and LeDoux 2007).
Syndemics and the Ecological Model
It is important to recognize that disease risk is not spread evenly within or between populations. Diseases combine and interact to create a syndemic, where the coexistence of two or more conditions exacerbates the effects of one or all conditions. A syndemic (versus a pandemic, for example) takes into account social, political, economic, and environmental factors that increase risk for the clustering of two or more diseases (Singer et al. 2017). One of the first syndemics identified involved substance abuse, violence, and AIDS. In inner cities in the U.S., the health crisis around HIV/AIDS was related to tuberculosis, sexually transmitted infections, hepatitis, cirrhosis, infant mortality, drug abuse, suicide, and homicide. These were connected to poverty, homelessness, unemployment, poor nutrition, lack of social support, and social and ethnic inequality (Singer et al. 2017). Together, these factors and others, like health policy and unequal access to health care, form an ecological model of health and disease, one that moves beyond biology and medical intervention (Sallis et al. 2008).
The COVID-19 pandemic represents a syndemic in which systemic racism in the healthcare system, differential access to diagnosis and treatment, income, employment, housing, family structure, pre existing conditions, and public health policies combined to result in higher rates of infection and death for African Americans, Native Americans, Asians, and Hispanic populations in the United States (Figure 16.11).
| Rate ratios compared to White, Non-Hispanic persons | American Indian or Alaska Native, Non-Hispanic persons | Asian, Non-Hispanic persons | Black or African American, Non-Hispanic persons | Hispanic or Latino persons |
|---|---|---|---|---|
| Cases | 1.6x | .8x | 1.1x | 1.5x |
| Hospitalization | 2.7x | .8x | 2.3x | 2.0x |
| Death | 2.1x | .8x | 1.7x | 1.8x |
COVID-19 was the third leading cause of death in the U.S. in 2020 and 2021 (NIH 2022; Figure 16.12), but morbidity and mortality was not equally spread across the population. Working-class people and people of color in the U.S. are more likely to live in poverty, in areas with high rates of crime and violence, and in close proximity to freeways and environmental threats like petrochemical plants and waste incinerators (Singer and Baer 2012). Many such neighborhoods are also food “deserts” without ready access to a healthy, affordable diet, made more challenging by residents not owning a car (Food Empowerment Project n.d.). Low-income people also often lack access to high-quality health care and delay or avoid preventive care and health screenings (Ross et al. 2007). These factors contributed to higher rates of preexisting conditions, including obesity, diabetes, hypertension, asthma, heart disease, chronic obstructive pulmonary disease (COPD), and smoking behavior, which then led to more complications and higher death rates from COVID (Ghosh et al. 2021).
Family structure also affected COVID exposure and severity. Many Americans live in multigenerational households, including 27% of Hispanics, 29% of Asians, 26% of African Americans, and 20% of Whites (Cohn and Passel 2018). Not all multigenerational households are equal, however. Over twice as many African Americans as Whites are in multigenerational families in which at least one family member is unemployed, and over three times as many African Americans are in multigenerational families in which everyone is simultaneously unemployed (Park, Wiemers, and Seltzer 2019). Family members in multigenerational households were at a much higher risk of developing more severe forms of COVID due to decreased personal space and multiple exposures to the virus, as well as higher rates of diabetes, smoking, and residents living below the poverty line (Ghosh et al. 2021). While aimed at reducing overall infection rates from COVID, public health measures such as mandatory lockdowns only exacerbated the situation in overcrowded and multigenerational housing, resulting in higher rates of infection and death in these communities.
|
United States |
Worldwide |
|---|---|
|
1. Heart disease |
1. Heart disease |
|
2. Cancer |
2. Stroke |
|
3. COVID-19 |
3. COVID-19 |
|
4. Accidents |
4. Chronic Obstructive Pulmonary Disease |
|
5. Stroke |
5. Lower respiratory infections |
There is a long history of systemic racism and discrimination in the medical system in the United States (Washington 2006). African Americans have been subjected to medical testing and experimentation without their consent or knowledge since the time of slavery. They continue to routinely receive care of poorer quality than whites (Williams and Wyatt 2015), less pain medication during treatment and hospitalization (Green et al. 2003), and differential treatment during pregnancy and childbirth (Washington 2006). Many Americans, including 50% of White medical students and residents in one recent study (Hoffman et al. 2016), hold at least one false belief about African Americans, including “Black people’s skin is thicker than white people’s skin,” “Blacks have stronger immune systems than whites,” and “Blacks’ nerve endings are less sensitive than whites’.” Such beliefs affect health care for African Americans in medical emergencies and for chronic conditions.
During the COVID-19 pandemic, patients with darker skin in the United States were negatively affected by the very medical device most commonly used to assess oxygen levels in their blood. The pulse oximeter, a small device that clips onto the tip of your index finger and measures blood oxygen levels, experienced increased use in home, clinical, and hospital settings during the COVID-19 pandemic. Decisions regarding treatment and hospital admission for patients infected with COVID were often based on pulse oximeter readings (Valbuena, Merchant, and Hough 2022). The problem is the device overestimates oxygen saturation in patients with darker skin, an issue which has been recognized for over thirty years (Valbuena, Merchant, and Hough 2022). It would be as if a standard thermometer reported lower body temperatures for patients of color, making it seem as if they did not have a fever when they actually did. In the case of COVID-19, Asians, Hispanics, and African Americans experienced inaccurately high readings of their oxygen levels (with African Americans and darker-skinned Hispanics having the highest), resulting in delays in treatment, hospital admission, and access to medications to treat COVID and contributing to higher severity of illness and higher death rates among these populations in comparison to whites (Fawzi et al. 2022).
Employment was also a factor in unequal exposure to and death from COVID-19 (Raifman, Skinner, and Sojourner 2022), with many low-income workers making the choice (which, realistically, may not be a choice at all) to expose themselves to COVID in order to earn the funds necessary to purchase food, housing, and other necessities. Many such workers were then forced to miss work due to COVID infection. With only 35% of low-wage workers (as opposed to 95% of high-wage workers) having paid sick leave, this left many families struggling financially. Three years into the pandemic, low-wage workers continue to have the least access to COVID vaccines and boosters. The U.S. also lacks federal workplace-safety regulations with regard to vaccine and masking mandates that other nations enforce in times of high transmission, and it does not provide high-quality masks to its essential workers. Many occupations deemed essential by the CDC during the height of the pandemic—such as health care, emergency services, meat packing, agricultural work, teaching, and jobs in the hospitality sector—experienced higher rates of morbidity and mortality from COVID. Many of these fields disproportionately employ people of color (McKinsey and Company 2021). Given this, future policies that address the pandemic at a structural level—for example, providing monetary assistance to people who work in environments with a high risk of infection, such as cleaning, nursing, transportation, retail, restaurant work, and factory work, so that they can remain at home—may function more effectively to prevent transmission and curb future outbreaks (Arnot et al. 2020).
Food for Thought
This chapter focused primarily on health conditions prevalent in contemporary, industrialized societies that are due, in part, to the mismatch between our evolved biology and modern environments. These are the built environment and the social environment, which together form the obesogenic environment in which unhealthy behaviors are encouraged. This chapter will close by examining each of these in a college context.

Consider your campus from an evolutionary perspective. To what degree does the built environment lend itself to physical activity as part of daily life? Is your campus constructed in ways that promote driving at the expense of walking or biking? If driving is necessary, is parking available close to the buildings or do you need to walk a fair distance from the parking lot to your destination? Do the buildings have stairs or ramps or is it necessary to take the elevator? Is it possible to negotiate safely around campus on foot or by bike in all weather? After dark? How about the classrooms and computer labs? Do they have standing or treadmill desks? Does your class schedule encourage walking from building to building between classes, or are most courses in your major scheduled in the same location? Most college majors also lack a physical education requirement, leaving it up to students to incorporate exercise into already-challenging schedules (Figure 16.13).
Sociocultural factors that contribute to obesity include food advertising, ubiquitous fast-food and junk food options, and social pressure to consume, all of which are present on college campuses. Although nutrition on campuses has improved in recent years, many students find eating healthy in the dining halls and dorms challenging (Plotnikoff et al. 2015), and students who live off campus fare even worse (Small et al. 2013). There are also parties and other social events, a normal part of college life, that involve unhealthy food and encourage behaviors like alcohol consumption and smoking. Give some thought to the social atmosphere on your campus and the ways it may contribute to obesity. My own freshman orientation involved a succession of pizza parties, ice cream socials, and barbecues, followed by late-night runs to the nearest fast-food outlet. The purpose of these events was to encourage people to make friends and feel comfortable living away from home, but the foods served were unhealthy, and there was social pressure to join in and be part of the group. Such activities set students up for the “freshman fifteen” and then some. They also reinforce the idea that being social involves eating (and sometimes drinking and/or smoking).
Sedentarism and inactivity are also built into the academics of college life. Digital technology is a significant contributor to obesity. Students use laptops and cell phones to take notes, complete their work outside of class, and access social media. There are also video games, virtual reality headsets, and streaming television and movies for entertainment. The built environment of college already necessitates that students sit in class for hours each day, then sit at computers to complete work outside of class. The social environment enabled by digital technology encourages sitting around for entertainment. It is telling that we call it “binge watching” when we spend hours watching our favorite shows. Doing so often involves eating, as well as multiple exposures to food advertising embedded in the shows themselves. In these ways, college contributes to the development of obesity-causing behaviors that can have negative health ramifications long after college is over (Small et al. 2013).
In the U.S., the greatest increase in obesity is among young adults aged 18–29 years, a significant percentage of whom are college students (Plotnikoff et al. 2015). Analyses of college students’ behavior across semesters shows consumption of fruits and vegetables drops over time, as does the amount of physical activity, while consumption of sugar-sweetened beverages and fast-food goes up, leading to weight gain at nearly six times the rate of the general public (Small et al. 2013). In response, many colleges and universities have instituted programs to encourage healthier eating and more physical activity among students (Plotnikoff et al. 2015). It is important to emphasize that neither changes in diet or exercise are effective on their own.. A 2022 study of over 340,000 British participants demonstrated that physical activity and diet quality did not individually have an impact on cardiovascular disease or cancers (Ding et al. 2022). That is, hitting the gym won’t counteract the consequences of consuming high-calorie, fatty foods, and eating kale all day can’t cancel out sedentary habits.
Just as no one fad diet is going to prove healthier than another, no one type of exercise is better than another. Anything that raises your heart rate and that you enjoy doing for at least an hour each day will work. Take advantage of opportunities to build exercise into everyday life. Take the stairs, park as far away from buildings as possible, ride a bike or walk instead of driving, and take walks between classes instead of sitting down and checking your phone. As far as diets go, eating a few less unhealthy calories each day, one less soda, no sugar in your coffee, or letting that last slice of pizza go to someone else, make a difference in the long run. Little changes add up to bigger ones. We cannot change our biology, but we can certainly change our habits.
Review Questions
- Why do humans like foods that are “bad” for them? Describe the evolutionary underpinnings of our tastes for sugar, salt, and fat.
- How might understanding contemporary disease from an evolutionary perspective benefit medical practitioners in treating their patients?
- Several risk factors for conditions like heart disease, diabetes, and cancer are referred to as “lifestyle factors,” implying these are behavioral choices people make that put them at risk. These include unhealthy eating, lack of physical activity, smoking, and alcohol consumption. To what degree is unhealthy behavior structured by the physical and social environment? For example, how does being a college student influence your eating habits, physical activity patterns, smoking, and consumption of alcohol?
- Who benefits from the global obesity epidemic? Think about how the following industries and institutions might profit from it: The medical establishment? The fitness industry? The diet industry? Fashion? Pharmaceutical companies? Food manufacturers? Advertisers?
Key Terms
Body mass index (BMI): A person’s weight in kilograms divided by the square of their height in meters. This is the most widely used measure for identifying obesity. The formula using kilograms and meters (or centimeters) is: weight (kg) / [height (m)]2 . The formula using pounds and inches is: 703 x weight (lbs) / [height (in)]2 . Use of the BMI is controversial for several reasons, including that it does not take into account age, bone structure, muscle mass, fat distribution, or ethnic and racial differences in body type.
Cancer: A collection of related diseases in which some of the body’s cells begin to divide without stopping and spread into surrounding tissues.
Cardiovascular disease (CVD): A disease of the heart and blood vessels, often related to atherosclerosis. CVD is a condition in which a substance called plaque builds up in the walls of the arteries, the blood vessels that carry blood away from the heart, which compromises the flow of blood to the heart or brain.
Central nervous system: The complex of nerve tissues stemming from the brain and spinal cord that controls the activities of the body.
Circulatory (system): The biological system that circulates blood around the body via the heart, arteries, and veins, delivering oxygen and nutrients to organs and cells and carrying waste products away.
Diabetes mellitus: An endocrine disorder in which high glucose (blood sugar) levels occur over a prolonged period of time. Blood glucose is your body’s main source of energy and comes from the food you eat. Insulin, a hormone made by the pancreas, helps glucose from food get into your cells to be used for energy. Sometimes your body does not make enough—or any—insulin (type 1 diabetes) or does not take up insulin well (type 2 diabetes). Glucose then stays in your blood and does not reach your cells.
“Double burden”: Refers to parts of the world in which there is a prevalence of chronic disease (e.g., cancer, heart disease) while, at the same time, there are also high rates of infectious disease due to poverty, malnutrition, poor sanitation, and lack of access to health care, often accompanied by high rates of maternal and child mortality.
Ecological model: Ecological models of health and disease emphasize environmental and policy contexts of behavior, while incorporating social and psychological influences, rather than focusing on individual behaviors. These models encompass multiple levels of influence and can lend themselves to more comprehensive health interventions.
Emerging infectious diseases (EIDs): Infections that have recently appeared within a population or those whose incidence or geographic range is rapidly increasing or threatens to increase in the near future. Examples include Covid-19, Ebola, Zika, SARS, and avian (bird) flu.
Endocrine system: Those organs in the body whose primary function is the production of hormones.
Epidemiological transition: A transformation in patterns of disease (morbidity) and death (mortality) among a population.
Glycemic index (GI): A system that ranks foods on a scale from 1 to 100 based on their effect on blood-sugar levels. Carbohydrates with a low GI value (55 or less) are more slowly digested and metabolized causing a lower, slower rise in blood glucose and insulin levels.
Hypertension: High blood pressure. Blood pressure is the force exerted by the blood against the walls of the blood vessels. In a blood pressure reading, the top number (usually higher) refers to the systolic pressure, the amount of pressure in your arteries during the contraction of your heart muscle when your heart beats. The bottom number is the diastolic pressure when your heart muscle is resting between beats. Hypertension can lead to severe health complications and increases the risk of heart attack and stroke.
Incidence: The rate at which new cases of a disease occur in a population over a given period of time.
Insulin: A hormone produced in the pancreas that regulates the amount of glucose in the blood. Lack of insulin or the inability to absorb insulin causes diabetes.
Metabolic syndrome: A cluster of conditions, including increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels that occur together, increasing the risk of heart disease, stroke, and diabetes. Lifestyle changes like losing weight, exercising regularly, and making dietary changes can help prevent or reverse metabolic syndrome.
Menarche: The first occurrence of menstruation.
Morbidity: The number of cases of disease per unit of population occurring over a unit of time.
Mortality: The number of deaths attributable to a particular cause per unit of population over a unit of time.
Noncommunicable diseases (NCDs): Also known as chronic diseases, NCDs tend to be of long duration and are the result of a combination of genetic, physiological, environmental, and behavior factors. The main types of NCDs are cardiovascular diseases (like heart attacks and stroke), cancers, chronic respiratory diseases (such as chronic obstructive pulmonary disease and asthma), and diabetes.
Obesity: A medical condition in which excess body fat has accumulated to the point that it has adverse effects on health. Although controversial due to its lack of ethnic and racial specificity, the most widely used measure for identifying obesity is the body mass index (BMI), a person’s weight in kilograms divided by the square of their height in meters. A measure of 30 kg/m2 is considered obese and 25–29 kg/m2 is considered overweight. Distribution of body fat also matters. Fat in the abdominal region has a stronger association with type 2 diabetes and cardiovascular disease, meaning waist-to-hip ratio and waist circumference are also important indicators of obesity-related health risk.
Obesogenic: Promoting excessive weight gain.
Omnivorous: Able to eat and digest foods of both plant and animal origins.
Osteoarthritis: Refers to the degeneration of joint cartilage and underlying bone, causing pain and stiffness. In the absence of previous injury, it is most common in modern populations from middle age onward.
Prevalence: The proportion of individuals in a population who have a particular disease or condition at a given point in time.
Sedentarism: A way of life characterized by much sitting and little physical activity.
Sedentism: Living in groups settled permanently in one place.
Stress response: A predictable response to any significant threat to homeostasis. The human stress response involves the Central Nervous System and the endocrine system acting together. Sudden and severe stress incites the “flight or flight” response from the autonomic nervous system in conjunction with hormones secreted by the adrenal and pituitary glands, increasing our heart rate and breathing and releasing glucose from the liver for quick energy.
Stroke: A stroke occurs when a blood vessel leading to the brain is blocked or bursts, preventing that part of the brain from receiving blood and oxygen, leading to cell death.
Syndemic: The aggregation (grouping together) of two or more diseases or health conditions in a population in which there is some level of harmful biological or behavioral interface that exacerbates the negative health effects of any or all of the diseases involved. Syndemics involve the adverse interaction of diseases of all types, including infections, chronic noncommunicable diseases, mental health problems, behavioral conditions, toxic exposure, and malnutrition.
Tricep skinfold measurement: The triceps skinfold site is a common location used for the assessment of body fat using skinfold calipers. A section of skin on the posterior (back) surface of the arm that lays atop the tricep muscle is pinched between calipers. The resulting measurement is matched against a chart standardized for age and gender.
“Triple burden”: A fourth epidemiological transition currently underway in which some parts of the globe are suffering from the “double burden” of infectious and chronic diseases combined with injuries and diseases related to intensifying globalization, urbanization, deforestation, and climate change.
Vector-borne diseases: Human illnesses caused by parasites, viruses, and bacteria that are transmitted by mosquitoes, flies, ticks, mites, snails, and lice.
Zoonoses: Diseases that can be transmitted from animals to humans.
About the Author

Joylin Namie, Ph.D.
Truckee Meadows Community College, jnamie@tmcc.edu
Joylin Namie is Professor of Anthropology at Truckee Meadows Community College, where she teaches courses in biological and cultural anthropology. Her current research interest is in culturally and environmentally sustainable tourism in desert environments, particularly in the country of Jordan and the U.S. state of Nevada. She was awarded a fellowship to Jordan from the Council of American Overseas Research Centers (CAORC) in 2020 to explore this topic, including visiting Petra and other important tourism destinations in Jordan. Dr. Namie’s favorite things in life are teaching, competing in sports, and traveling.
For Further Exploration
Lents, Nathan H. 2018. Human Errors: A Panorama of Our Glitches, from Pointless Bones to Broken Genes. Boston: Houghton Mifflin Harcourt.
Stearns, Stephen C., and Jacob C. Koella, eds. 2008. Evolution in Health and Disease. 2nd edition. United Kingdom: Oxford University Press.
Zuk, Marlene. 2013. Paleofantasy: What Evolution Really Tells Us about Sex, Diet, and How We Live. New York: W. W. Norton & Company.
References
Abid, Zaynah, Amanda J. Cross, and Rashmi Sinha. 2014. “Meat, Dairy, and Cancer.” The American Journal of Clinical Nutrition 100 (S1): 386S–393S.
Akil, Luma, and H. Anwar Ahmad. 2011. “Relationships between Obesity and Cardiovascular Diseases in Four Southern States and Colorado.” Journal of Health Care for the Poor and Underserved 22 (S4): 61–72.
Ali, Aus Tariq. 2014. “Reproductive Factors and the Risk of Endometrial Cancers.” International Journal of Gynecological Cancer 24 (3): 384–393.
American Heart Association. 2018. “Heart Disease and Stroke Statistics-2018 Update: A Report.” Circulation 137 (12). Accessed April 7, 2023. https://www.ahajournals.org/doi/10.1161/cir.0000000000000558.
American Psychiatric Association (APA). 2013. Diagnostic and Statistical Manual of Mental Disorder. 5th Edition: DSM-5. Washington, DC: APA.
Armelagos, George J. 1990. “Health and Disease in Prehistoric Populations in Transition.” Disease in Populations in Transition: Anthropological and Epidemiological Perspectives, edited by George J. Armelagos and Alan C. Swedland, 127–144. New York: Bergin & Garvey.
Armelagos, George J., Peter J. Brown, and Bethany Turner. 2005. “Evolutionary, Historical and Political Economic Perspectives on Health and Disease.” Social Science and Medicine 61 (4): 755-765.
Arnot, Megan, Eva Brandl, O. L. K. Campbell, Yuan Chen, Mark Dyble, Emily H. Emmott, et al. 2020. Evolution, Medicine, and Public Health 2020 (1): 264–278. https://doi.org/10.1093/emph/eoaa038.
Asher, Claire. 2017. “Illegal Bushmeat Trade Threatens Human Health and Great Apes.” Mongabay, April 6. Accessed April 4, 2023. https://news.mongabay.com/2017/04/illegal-bushmeat-trade-threatens-human-health-and-great-apes/.
Baker, W. A., G. A. Hitman, K. Hawrami, M .I. McCarthy, A. Riikonen, E. Tuomilehto-Wolf, A. Nissinen, et al. 1994. “Apolipoprotein D Gene Polymorphism: A New Genetic Marker for Type 2 Diabetic Subjects in Nauru and South India.” Diabetic Medicine 11 (10): 947–952.
Baltic, Milan Z., and Marija Boskovic. 2015. “When Man Met Meat: Meat in Human Nutrition from Ancient Times Till Today.” Procedia Food Science 5: 6- 9.
Blue Cross Blue Shield Association (BCBSA). 2017. “Diabetes and the Commercially Insured U.S. Population.” The Health of America Report, August 1. Accessed April 4, 2023. https://www.bcbs.com/the-health-of-america/reports/diabetes-and-commercially-insured-us-population.
Bogin, Barry. 1991. “The Evolution of Human Nutrition.” In The Anthropology of Medicine: From Culture to Method, edited by Lola Romanucci-Ross, Daniel E. Moerman, and Laurence R. Tancredi, 158–195. New York: Bergin & Garvey.
Bouchard, Claude. 2007. “The Biological Predisposition to Obesity: Beyond the Thrifty Genotype Scenario.” International Journal of Obesity 31 (9): 1337–1339.
Buchman, Aron S., Lei Yu, Robert S. Wilson, Andrew Lim, Robert J. Dawe, Chris Gaiteri, Sue E. Leurgans, Julie A. Schneider, and David A. Bennett. 2019. “Physical Activity, Common Brain Pathologies, and Cognition in Community-Dwelling Older Adults.” Neurology 98 (2). http://doi.org/10.1212/WNL.0000000000006954.
Centers for Disease Control and Prevention (CDC). N.d. “Global Health – Pakistan.” Accessed April 4, 2023. https://www.cdc.gov/globalhealth/countries/pakistan/default.htm.
Centers for Disease Control and Prevention (CDC). 2014. “Breastfeeding Report Card: United States/2014.” Atlanta, GA: Centers for Disease Control and Prevention.
Centers for Disease Control and Prevention (CDC). 2020. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States. Accessed April 7, 2023 from https://diabetesresearch.org/wp-content/uploads/2022/05/national-diabetes-statistics-report-2020.pdf.
Centers for Disease Control and Prevention (CDC). 2022. “CDC Releases Updated Maps of America’s High Levels of Inactivity.” January 20. https://www.cdc.gov/media/releases/2022/p0120-inactivity-map.html.
Cerón, Ella. 2017. “Here’s Every Oreo Flavor Ever Created.” TeenVogue.com, June 19. Accessed April 4, 2023. https://www.teenvogue.com/story/every-oreo-flavor-ranked.
Chin, Jessie, Brennan R. Payne, Wai-Tat Fu, Daniel G. Morrow, and Elizabeth A. L. Stine-Morrow. 2015. “Information Foraging across the Life Span: Search and Switch in Unknown Patches.” Topics in Cognitive Science 7 (3): 428–450.
Cohn, D’Vera, and Jeffrey S. Passel. 2018. “A Record 64 Million Americans Live In Multigenerational Households.” Pew Research Center, April 5. Accessed April 4, 2023. https://www.pewresearch.org/fact-tank/2018/04/05/a-record-64-million-americans-live-in-multigenerational-households/.
Cooling, Laura. 2015. “Blood Groups in Infection and Host Susceptibility.” Clinical Microbiology Reviews 28 (3): 801–870.
Croston, Glenn. 2012. “The Thing We Fear More Than Death: Why Predators Are Responsible for Our Fear of Public Speaking.” Psychology Today blog, November 29. Accessed April 4, 2023. https://www.psychologytoday.com/us/blog/the-real-story-risk/201211/the-thing-we-fear-more-death.
Currie, Candace, Naman Ahluwalia, Emmanuelle Godeau, Saoirse Nic Gabhainn, Pernille Due, and Dorothy B. Mille. 2012. “Is Obesity at Individual and National Level Associated with Lower Age at Menarche? Evidence from 34 Countries in the Health Behaviour in School-Aged Children Study.” Journal of Adolescent Health 50 (6): 621–626.
David, A. Rosalie, and Michael Zimmerman. 2010. “Cancer: An Old Disease, A New Disease or Something In Between?” Nature Reviews: Cancer 10 (10): 728–733.
Davis, Mike. 2005. The Monster at Our Door: The Global Threat of Avian Flu. New York: Owl Books.
de Silva, A. M., K. R. Walder, T. J. Aitman, T. Gotoda, A. P. Goldstone, A. M. Hodge, M. P. de Courten, P. Z. Zimmet, and G. R. Collier. 1999. “Combination of Polymorphisms in OB-R and the OB Gene Associated with Insulin Resistance in Nauruan Males.” International Journal of Obesity 23 (8): 816–822.
Dimsdale, Joel E. 2008. “Psychological Stress and Cardiovascular Disease.” Journal of the American College of Cardiology 51 (13): 1237–1246.
Ding, Ding, Joe Van Buskirk, Binh Nguyen, Emmanuel Stammotakis, Mona Elbarbary, Nicole Veronese, Philip J. Clare, et al. 2022. “Physical Activity, Diet Quality and All-Cause Cardiovascular Disease and Cancer Mortality: A Prospective Study of 346,627 UK Biobank Participants.” British Journal of Sports Medicine 56 (20): 1148–1156.
Dutton, Denis. 2009. The Art Instinct: Beauty, Pleasure, and Human Evolution. New York: Bloomsbury.
Eaton, S. Boyd, Melvin Konner, and Marjorie Shostak. 1988. “Stone Agers in the Fast Lane: Chronic Degenerative Diseases in Evolutionary Perspective.” American Journal of Medicine 84 (4): 739–749.
Eaton, S. Boyd, Malcolm C. Pike, Roger V. Short, Nancy C. Lee, James Trussell, Robert A. Hatcher, James W. Wood, et al. 1994. “Women’s Reproductive Cancers in Evolutionary Context.” The Quarterly Review of Biology 69 (3): 353–367.
Ewald, Paul W. 2018. “Ancient Cancers and Infection-Induced Oncogenesis.” International Journal of Paleopathology 21: 178–185. http://dx.doi.org/10.1016/J.ijpp.2017.08.007.
Farb, Peter, and George Armelagos. 1980. Consuming Passions: The Anthropology of Eating. New York: Washington Square Press.
Fawzi, Ashraf, Tianshi David Wu, Kunbo Wang, Matthew L. Robinson, Jad Farha, Amanda Bradke, Sherita H. Golden, et al. 2022. “Racial and Ethnic Discrepancy in Pulse Oximetry and Delayed Identification of Treatment Eligibility among Patients With COVID-19.” JAMA Internal Medicine 182 (7): 730–738.
Flinn, Mark V., and Barry G. England. 2003. “Childhood Stress: Endocrine and Immune Responses to Psychosocial Events.” In Social and Cultural Lives of Immune Systems: Theory and Practice in Medical Anthropology and International Health, edited by James M. Wilce Jr., 105–146. London: Routledge.
Food Empowerment Project. N.d. “Food Deserts.” Accessed April 4, 2023. https://foodispower.org/access-health/food-deserts/.
Gao, George. 2015. “Americans’ Ideal Family Size Is Smaller Than It Used to Be.” Pew Research Center, May 8. Accessed April 4, 2023. http://www.pewresearch.org/fact-tank/2015/05/08/ideal-size-of-the-american-family/.
Ghosh, A. K., S. Venkatraman, O. Soroka, E. Reshetnyak, M. Rajan, A. An, J. K. Chae, et al. 2021. “Association between Overcrowded Households, Multigenerational Households, and COVID-19: A Cohort Study.” Public Health 198: 273–279.
Government of Pakistan. “Pakistan: Updated Nationally Determined Contributions.” 2021. Accessed October 12, 2022. https://unfccc.int/sites/default/files/NDC/2022-06/Pakistan%20Updated%20NDC%202021.pdf.
Greaves, Mel. 2015. “Evolutionary Determinants of Cancer.” Cancer Discovery 5 (8): 806–820.
Green, Carmen R., Karen O. Anderson, Tamara A. Baker, Lisa C. Campbell, Sheila Decker, Robert B. Fillingim, Donna A. Kalukalani, et al. 2003. “The Unequal Burden of Pain: Confronting Racial and Ethnic Disparities in Pain.” Pain Medicine 4 (3): 277–294.
Greenspan, Louise, and Julianna Deardorff. 2014. The New Puberty: How to Navigate Early Development in Today’s Girls. New York: Rodale.
Hamilton, Cheryl. 2011. Communicating for Results, a Guide for Business and the Professions, 9th Edition. Belmont, CA: Thomson Wadsworth.
Harper, Kristin, and George Armelagos. 2010. “The Changing Disease-Scape in the Third Epidemiological Transition.” International Journal of Environmental Research and Public Health 7 (2): 675–697.
Hoffman, Kelly M., Sophie Trawalter, Jordan R. Axt, and M. Norman Oliver. 2016. “Racial Bias in Pain Assessment and Treatment Recommendations, and False Beliefs about Biological Differences among Blacks and Whites.” PNAS 113 (16): 4296–4301.
International Agency for Research on Cancer (IARC). 2018. Red Meat and Processed Meat IARC Monographs on the Evaluation of Carcinogenic Risks to Humans, Volume 114. ISBN-13: 978-92-832-0152-6.
International Diabetes Federation (IDF). 2022. IDF Diabetes Atlas 2022 Reports. 10th edition. https://diabetesatlas.org/.
Jain, H. K. 2012. “Transition to Twenty-First Century Agriculture: Change of Direction.” Agricultural Research 1 (1): 12–17.
Jones, Kate E., Nikkita G. Patel, Mark A. Levy, Adam Storeygard, Deborah Balk, John L. Gittleman, and Peter Daszak. 2008. “Global Trends in Emerging Infectious Disease.” Nature 451 (7181): 990–993.
Karn, Mitesh, and Muna Sharma. 2021. “Climate Change, Natural Calamities, and the Triple Burden of Disease.” Nature Climate Change 11: 796–797.
Larsen, Clark Spencer. 2014. “Foraging to Farming Transition: Global Health Impacts, Trends, and Variation.” In Encyclopedia of Global Archaeology, edited by Claire Smith, 2818–2824. New York: Springer.
Lee, Richard B. 2013. The Dobe Ju/’hoansi. 4th edition. Belmont, CA: Wadsworth/Cengage Learning.
Lieberman, Daniel E. 2015. “Human Locomotion and Heat Loss: An Evolutionary Perspective.” Comprehensive Physiology 5 (1): 99–117.
Lieberman, Leslie Sue. 2006. “Evolutionary and Anthropological Perspectives on Optimal Foraging in Obesogenic Environments.” Appetite 47 (1): 3–9.
Liu, Gang. 2018. “Abstract P184: Meat Cooking Methods and Risk of Hypertension: Results From Three Prospective Cohort Studies.” Circulation 137 (S1): AP184.
Liu, Gang, Geng Zong, Kana Wu, Yang Hu, Yanping Li, Walter C. Willett, David M. Eisenberg, Frank B. Hu, and Qi Sun. 2018. “Meat Cooking Methods and Risk of Type 2 Diabetes: Results from Three Prospective Cohort Studies.” Diabetes Care 41 (5): 1049–1060.
Livingston, Gretchen. 2015. “Childlessness.” Pew Research Center, May 7. Accessed April 4, 2023. http://www.pewsocialtrends.org/2015/05/07/childlessness/.
Lucock, Mark D., Charlotte E. Martin, Zoe R. Yates, and Martin Veysey. 2014. “Diet and Our Genetic Legacy in the Recent Anthropocene: A Darwinian Perspective to Nutritional Health.” Journal of Evidence-Based Complementary and Alternative Medicine 19 (1): 68–83.
Mandsager, Kyle, Serge Harb, and Paul Cremer. 2018. “Association of Cardiorespiratory Fitness with Long-term Mortality among Adults Undergoing Exercise Treadmill Testing.” JAMA Network Open 1 (6): e183605. http://doi.org/10.1001/jamanetworkopen.2018.3605.
Marciniak, Stephanie, and George H. Perry. 2017. “Harnessing Ancient Genomes to Study the History of Human Adaptation.” Nature Reviews Genetics 18: 659–674.
Marlowe, Frank W. 2005. “Hunter-Gatherers and Human Evolution.” Evolutionary Anthropology 14 (2): 54–67.
Marmot, Michael. 2005. “Social Determinants of Health Inequality.” The Lancet 365 (9464): 1099–1104.
Martini, Frederic H., William C. Ober, Edwin F. Bartholomew, and Judi L. Nath. 2013. Visual Essentials of Anatomy & Physiology. Boston, MA: Pearson.
Mathews, T. J., and Brady E. Hamilton. 2016. “Mean Age of Mothers Is on the Rise: United States, 2000–2014.” National Center for Health Statistics (CHS) Data Brief. No. 232. Accessed April 4, 2023. https://www.cdc.gov/nchs/data/databriefs/db232.pdf.
McClellan, James E., and Harold Dorn. 2006. Science and Technology in World History: An Introduction. 2nd edition. Baltimore, MD: The Johns Hopkins University Press.
McElroy, Ann, and Patricia Townsend. 2009. Medical Anthropology in Ecological Perspective. 5th edition. Boulder, CO: Westview Press.
McKee, Trudy, and James R. McKee. 2015. Biochemistry: The Molecular Basis of Life. 6th edition. Oxford, UK: Oxford University Press.
McKinsey and Company. 2021. “Race in the Workplace: Black Workers in the U.S. Private Sector.” February 21. Accessed April 4, 2023. https://www.mckinsey.com/featured-insights/diversity-and-inclusion/race-in-the-workplace-the-black-experience-in-the-us-private-sector.
Moss, Michael. 2013. Salt, Sugar, Fat: How the Food Giants Hooked Us. New York: Random House.
National Institutes of Health (NIH). 2022. “COVID-19 Was Third Leading Cause of Death in the United States in Both 2020 and 2021.” Media Advisory. July 5. Accessed April 4, 2023. https://www.nih.gov/news-events/news-releases/covid-19-was-third-leading-cause-death-united-states-both-2020-2021.
National Institutes of Health (NIH). 2017. “Obesity and Cancer Fact Sheet.” Last modified January, 2017. Accessed April 4, 2023. https://www.cancer.gov/about-cancer/causes-prevention/risk/obesity/obesity-fact-sheet.
Odes, Edward J., Patrick S. Randolph-Quinney, Maryna Steyn, Zach Throckmorton, Jacqueline S. Smilg, Bernhard Zipfel, Tanya N. Augustine, et al. 2016. “Earliest Hominin Cancer: 1.7-Million-Year-Old Osteosarcoma from Swartkrans Cave, South Africa.” South African Journal of Science 112 (7–8): 1–5.
Omran, Abdel R. 2005. “The Epidemiologic Transition: A Theory of the Epidemiology of Population Change.” The Milbank Quarterly, December 83 (4): 731-757. Accessed April 7, 2023. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2690264/.
Palma-Gudiel, H., A. Córdova-Palomera, E. Eixarch, M. Deuschle, and L. Fañanás. 2015. “Maternal Psychosocial Stress during Pregnancy Alters the Epigenetic Signature of the Glucocorticoid Receptor Gene Promoter in Their Offspring: A Meta-Analysis.” Epigenetics 10 (10): 893–902.
Park, Sung S., Emily E. Wiemers, and Judith A. Seltzer. 2019. “The Family Safety Net of Black and White Multigenerational Families.” Population and Development Review 45 (2): 351–378.
Pierce, Mary, and Rebecca Hardy. 2012. “Commentary: The Decreasing Age of Puberty—As Much a Psychosocial as Biological Problem?” International Journal of Epidemiology 41 (1): 300–302.
Plotnikoff, Ronald C., Sarah A. Costigan, Rebecca L. Williams, Melinda J. Hutchesson, Sarah G. Kennedy, Sara L. Robards, Jennifer Allen, Clare E. Collins, Robin Callister, and John Germov. 2015. “Effectiveness of Interventions Targeting Physical Activity, Nutrition and Healthy Weight for University and College Students: A Systematic Review and Meta-analysis.” International Journal of Behavioral Nutrition and Physical Activity 12 (1): 1–10.
Poinar, George. 2018. “Vertebrate Pathogens Vectored by Ancient Hematophagous Arthropods.” Historical Biology, November 7. http://doi.org/10.1080/08912963.2018.1545018.
Pontzer, Herman, David A. Raichlen, Brian M. Wood, Audax Z. P. Mabulla, Susan B. Racette, and Frank W. Marlowe. 2012. “Hunter-Gatherer Energetics and Obesity.” PLoS ONE 7 (7): e40503. http://doi.org/10.1371/journal.pone.0040503.
Pritchard, Jonathan K. 2010. “How We Are Evolving.” Scientific American 303 (4): 4047.
Raichlen, David A., and Gene E. Alexander. 2014. “Exercise, APOE Genotype, and the Evolution of the Human Lifespan.” Trends in Neurosciences 37 (5): 247–255.
Raichlen, David A., Herman Pontzer, Jacob A. Harris, Audax Z. P. Mabulla, Frank W. Marlowe, J. Josh Snodgrass, Geeta Eick, J. Colette Berbesque, Amelia Sancilio, and Brian M. Wood. 2016. “Physical Activity Patterns and Biomarkers of Cardiovascular Disease Risk in Hunter-Gatherers.” American Journal of Human Biology 29 (2): e22919. https://doi.org/10.1002/ajhb.22919.
Raifman, Julia, Alexander Skinner, and Aaron Sojourner. 2022. “The Unequal Toll of COVID-19 On Workers.” Working Economics Blog (of the Economic Policy Institute), February 7. Accessed April 4, 2023. https://www.epi.org/blog/the-unequal-toll-of-covid-19-on-workers/.
Randolph-Quinney, Patrick S., Scott A. Williams, Maryna Stein, Mark R. Meyer, Jacqueline S. Smilg, Steven E. Churchill, Edward J. Odes, Tanya Augustine, Paul Tafforeau and Lee Berger. 2016. “Osteogenic Tumour in Australopithecus sediba: Earliest Hominin Evidence for Neoplastic Disease.” South African Journal of Science 112 (7-8). Accessed April 7, 2023. http://www.scielo.org.za/scielo.php?script=sci_arttext&pid=S0038-23532016000400013. http://dx.doi.org/10.17159/sajs.2016/20150470
Rankinen, Tuomo, Aamir Zuberi, Yvon C. Chagnon, S. John Weisnagel, George Argyropoulos, Brandon Walts, Louis Pérusse, and Claude Bouchard. 2006. “The Human Obesity Gene Map: The 2005 Update.” Obesity 14 (4): 529–644.
Richards, M. P. 2002. “A Brief Review of the Archaeological Evidence for Palaeolithic and Neolithic Subsistence.” European Journal of Clinical Nutrition 56 (12): 1270–1278.
Ross, Joseph S., Susannah M. Bernheim, Elizabeth H. Bradley, Hsun-Mei Teng, and William T. Gallo. 2007. “Use of Preventive Care by the Working Poor in the United States.” Preventive Medicine 44 (3): 254–259.
Sallis, James F., Neville Owen, and Edwin B. Fisher. 2008. “Chapter 20: Ecological Models of Health Behavior.” In Health Behavior and Health Education: Theory, Research, and Practice, edited by Karen Glanz, Barbara K. Rimer, and K. Viswanath, 465–485. 4th edition. San Francisco, CA: Jossey-Bass.
Sharp, Paul M., and Beatrice H. Hahn. 2011. “Origins of HIV and the AIDS Pandemic.” Cold Springs Harbor Perspectives in Medicine 1 (1): a006841.
Sheerazi, Hadia A. 2022. “The Flood Seen from Space: Pakistan’s Apocalyptic Crisis.” State of the Planet (news from the Columbia Climate School), September 12. Accessed April 4, 2023. https://news.climate.columbia.edu/2022/09/12/the-flood-seen-from-space-pakistans-apocalyptic-crisis/.
Shiels, Meredith S., Anika T. Haque, Amy Berrington de González, and Neal D. Freedman. 2022. “Leading Causes of Death in the US During the COVID-19 Pandemic, March 2020 to October 2021.” JAMA 182 (8): 883-886. doi:10.1001/jamainternmed.2022.2476.
Shonkoff, Jack P., and Andrew S. Garner. 2012. “The Lifelong Effects of Early Childhood Adversity and Toxic Stress.” Pediatrics 129 (1): e232–e246. https://doi.org/10.1542/peds.2011-2663.
Singer, Merrill, and Hans Baer. 2012. “Health Disparity, Health Inequality.” In Introducing Medical Anthropology: A Discipline in Action, 2nd edition, edited by Merrill Singer and Hans Baer, 175–205. Lanham, MD: AltaMira.
Singer, Merrill, Nicola Bulled, Bayla Ostrach, and Emily Mendenhall. 2017. “Syndemics and the Biosocial Conception of Health.” Lancet 389 (10072): 941–950.
Small, Meg, Lisa Bailey-Davis, Nicole Morgan, and Jennifer Maggs. 2013. “Changes in Eating and Physical Activity Behaviors across Seven Semesters of College: Living On or Off Campus Matters.” Health Education and Behavior 40 (4): 435–441.
Smith-Morris, Carolyn M. 2004. “Reducing Diabetes in Indian Country: Lessons from the Three Domains Influencing Pima Diabetes.” Human Organization 63 (1): 34–46.
Sonfield, Adam, Kinsey Hasstedt, Megan L. Cavanaugh, and Ragnar Anderson. 2013. “The Social and Economic Benefits of Women’s Ability to Determine Whether and When to Have Children.” Report, March 13. New York: Guttmacher Institute. Accessed April 4, 2023. https://www.guttmacher.org/report/social-and-economic-benefits-womens-ability-determine-whether-and-when-have-children.
St. Pierre, Danielle. 2018. “The 15 Best Potato Chips for Every Flavor Craving.” Best, April 6. Accessed June 13, 2018. https://www.bestproducts.com/eats/food/g972/best-potato-chips/.
Stearns, Stephen C., Randolph M. Nesse, and David Haig. 2008. “Introducing Evolutionary Thinking into Medicine.” In Evolution in Health and Disease, edited by Stephen C. Stearns and Jacob C. Koella, 3–15. United Kingdom: Oxford University Press.
Strassmann, Beverly I. 1997. “The Biology of Menstruation in Homo Sapiens: Total Lifetime Menses, Fecundity, and Nonsynchrony in a Natural-Fertility Population.” Current Anthropology 38 (1): 123–129.
Strassmann, Beverly I. 1999. “Menstrual Cycling and Breast Cancer: An Evolutionary Perspective.” Journal of Women’s Health 8 (2): 193–202.
Trafialek, Joanna, and Wojciech Kolanowski. 2014. “Dietary Exposure to Meat-Related Carcinogenic Substances: Is There a Way to Estimate the Risk?” International Journal of Food Sciences and Nutrition 65 (6): 774–780.
Troeger, Christopher. 2023. “Just How Do Deaths Due to COVID-19 Stack Up?” Think Global Health. February 15. Accessed April 8, 2023. https://www.thinkglobalhealth.org/article/just-how-do-deaths-due-covid-19-stack#:~:text=Looking%20at%20official%20statistics%20alone,since%20the%20beginning%20of%202020.
Valbuena, Valeria S.M., Raina M. Merchant, and Catherine L. Hough. 2022. “Racial and Ethnic Bias in Pulse Oximetry and Clinical Outcomes.” Editorial. JAMA Internal Medicine 182 (7): 699–700.
Ventola, C. Lee. 2015. “The Antibiotic Resistance Crisis: Part I: Causes and Threats.” Pharmacy & Therapeutics 40 (4): 277–283.
Versini, Mathilde, Pierre-Yves Jeandel, Tomer Bashi, Giorgia Bizzaro, Miri Blank, and Yahuda Shoenfeld. 2015. “Unraveling the Hygiene Hypothesis of Helminthes and Autoimmunity: Origins, Pathophysiology, and Clinical Applications.” BMC Medicine, 13: 81. https://doi.org/10.1186/s12916-015-0306-7.
Vucenik, Ivana, and Joseph P. Stains. 2012. “Obesity and Cancer Risk: Evidence, Mechanisms, and Recommendations.” Special issue, “Nutrition and Physical Activity in Aging, Obesity, and Cancer,” Annals of the New York Academy of Sciences 1271 (1): 37–43.
Walker, Polly, Pamela Rhubart-Berg, Shawn McKenzie, Kristin Kelling, and Robert S. Lawrence. 2005. “Public Health Implications of Meat Production and Consumption.” Public Health Nutrition 8 (4): 348–356.
Washington, Harriet A. 2006. Medical Apartheid: The Dark History of Medical Experimentation on Black Americans from Colonial Times to the Present. New York: Anchor Books.
Williams, David R., and Selina A. Mohammed. 2013. “Racism and Health I: Pathways and Scientific Evidence.” American Behavioral Scientist 57 (8). http://doi.org/10.1177/0002764213487340.
Williams, David R., and Ronald Wyatt. 2015. “Racial Bias in Health Care and Health: Challenges and Opportunities.” JAMA 314 (6): 555–556. http://doi.org10.1001/jama.2015.9260.
Wolfe, Nathan, Claire P. Dunavan, and Jared Diamond. 2012. “Origins Of Major Human Infectious Diseases.” In Institute of Medicine: Improving Food Safety through a One Health Approach: Workshop Summary, A16. Washington, DC: National Academies Press. Accessed April 4, 2023. https://www.ncbi.nlm.nih.gov/books/NBK114494/.
World Health Organization (WHO). 2016. Global Report on Diabetes. Accessed April 4, 2023. http://apps.who.int/iris/bitstream/handle/10665/204871/9789241565257_eng.pdf.
World Health Organization (WHO). 2017. “Obesity and Overweight.” Fact Sheet. Last modified June 9, 2021; accessed April 4, 2023. http://www.who.int/mediacentre/factsheets/fs311/en/.
World Health Organization (WHO). 2018. “Cancer.” Fact Sheet. Last modified February 3, 2022; accessed April 5, 2023. http://www.who.int/news-room/fact-sheets/detail/cancer.
Worobey, Michael, Joshua I. Levy, Lorena Malpica Serrano, Alexander Crits-Christoph, Jonathan E. Pekar, Stephan A. Goldstein, Angela L. Rassmussen, et al. July 26, 2022. “The Huanan Seafood Wholesale Market in Wuhan was the Early Epicenter of the COVID-19 Pandemic.” SCIENCE 26 (377): 951–959. http://doi.org/10.1126/science.abp8715.
Worthman, Carol M., and Jennifer Kuzara. 2005. “Life History and the Early Origins of Health Differentials.” American Journal of Human Biology 17 (1): 95–112.
Wrangham, Richard. 2009. Catching Fire: How Cooking Made Us Human. New York: Basic Books.
Yehuda, Rachel, and Joseph LeDoux. 2007. “Response Variation Following Trauma: A Translational Neuroscience Approach to Understanding PTSD.” Neuron 56 (1): 19–32.
Zuckerman, Molly K., and George J. Armelagos. 2014. “The Hygiene Hypothesis and the Second Epidemiologic Transition.” In Modern Environments and Human Health: Revisiting the Second Epidemiologic Transition, edited by Molly K. Zuckerman, 301–320. Hoboken, NJ: Wiley-Blackwell.
Zuckerman, Molly Kathleen, Kristin Nicole Harper, Ronald Barrett, and George John Armelagos. 2014. “The Evolution of Disease: Anthropological Perspectives on Epidemiologic Transitions.” Special issue, “Epidemiological Transitions: Beyond Omran’s Theory,” Global Health Action 7 (1): 23303. http://doi.org/10.3402/gha.v7.23303.
Figure Description
Figure 16.4: Obesity rates by country, 2017. The following are the rates as percentages of the total population of these countries:
- Japan, 3.7%
- India, 5%
- Korea, 5.3%
- Indonesia, 5.7%
- China, 7%
- Italy, 9.8%
- Switzerland, 10.2%
- Austria, 14.7%
- France, 15.3%
- Poland, 16.7%
- Spain, 16.7%
- Greece, 17%
- Israel, 17.8%
- Iceland, 19%
- Russian Federation, 19.6%
- Brazil, 20.8%
- Columbia, 20.9%
- Ghana, 22%
- Turkey, 22.3%
- Iceland, 23%
- Germany, 23.6%
- Costa Rica, 24.4%
- Finland, 24.8%
- Chile, 25.1%
- Canada, 25.8%
- South Africa, 26.5%
- United Kingdom, 26.9%
- Australia, 26.9%
- Mexico, 27.9%
- United States, 38.2%
- Egypt, 39%
Figure 16.10: This chart depicts decreasing ages at time of first menstruation (menarche) in seven countries:
- In Germany/Finland, the age of menarche was approximately 16.5 years in 1860. This dropped to approximately 13.5 years by 1940.
- In Norway, the age of menarche was approximately 17 years of age in 1850. This dropped to approximately 13.3 by 1950, where it remained for 30 more years.
- In Sweden, the age of menarche was approximately 15.7 in 1890, dropping to approximately 14 years by 1950.
- There appears to be less data for Denmark. For Denmark, menarche was 13.7 in 1950 and dropped to approximately 13.3 by 1960.
- In the US, the age of menarche was 14 years in 1905. This dropped to 11 by 1990. This is the lowest data point on the chart.
- In the UK, the age of menarche was 13.3 in 1945, dropping to approximately 12.7 by 1970.
The number of cases of disease per unit of population occurring over a unit of time.
The number of deaths attributable to a particular cause per unit of population over a unit of time.
A transformation in patterns of disease (morbidity) and death (mortality) among a population.
A medical condition in which excess body fat has accumulated to the point that it has adverse effects on health. Although controversial due to its lack of ethnic and racial specificity, the most widely used measure for identifying obesity is the body mass index (BMI), a person’s weight in kilograms divided by the square of their height in meters. A measure of 30 kg/m2 is considered obese and 25–29 kg/m2 is considered overweight. Distribution of body fat also matters. Fat in the abdominal region has a stronger association with type 2 diabetes and cardiovascular disease, meaning waist-to-hip ratio and waist circumference are also important indicators of obesity-related health risk.
A collection of related diseases in which some of the body’s cells begin to divide
without stopping and spread into surrounding tissues.
Able to eat and digest foods of both plant and animal origins.
High blood pressure. Blood pressure is the force exerted by the blood against the walls of the blood vessels. In a blood pressure reading, the top number (usually higher) refers to the systolic pressure, the amount of pressure in your arteries during the contraction of your heart muscle when your heart beats. The bottom number is the diastolic pressure when your heart muscle is resting between beats. Hypertension can lead to severe health complications and increases the risk of heart attack and stroke.
A disease of the heart and blood vessels, often related to atherosclerosis. CVD is a condition in which a substance called plaque builds up in the walls of the arteries, the blood vessels that carry blood away from the heart, which compromises the flow of blood to the heart or brain.
Diseases that can be transmitted from animals to humans.
Human illnesses caused by parasites, viruses, and bacteria that are transmitted by mosquitoes, flies, ticks, mites, snails, and lice.
The triceps skinfold site is a common location used for the assessment of body fat using skinfold calipers. A section of skin on the posterior (back) surface of the arm that lays atop the tricep muscle is pinched between calipers. The resulting measurement is matched against a chart standardized for age and gender.
Refers to the degeneration of joint cartilage and underlying bone, causing pain and stiffness. In the absence of previous injury, it is most common in modern populations from middle age onward.
A way of life characterized by much sitting and little physical activity.
Also known as chronic diseases, NCDs tend to be of long duration and are the result of a combination of genetic, physiological, environmental, and behavior factors. The main types of NCDs are cardiovascular diseases (like heart attacks and stroke), cancers, chronic respiratory diseases (such as chronic obstructive pulmonary disease and asthma), and diabetes.
Refers to parts of the world in which there is a prevalence of chronic disease (e.g., cancer, heart disease) while, at the same time, there are also high rates of infectious disease due to poverty, malnutrition, poor sanitation, and lack of access to health care, often accompanied by high rates of maternal and child mortality.
Infections that have recently appeared within a population or those whose incidence or geographic range is rapidly increasing or threatens to increase in the near future. Examples include Covid-19, Ebola, Zika, SARS, and avian (bird) flu.
A fourth epidemiological transition currently underway in which some parts of the globe are suffering from the “double burden” of infectious and chronic diseases combined with injuries and diseases related to intensifying globalization, urbanization, deforestation, and climate change.
The proportion of individuals in a population who have a particular disease or condition at a given point in time.
Promoting excessive weight gain.
Those organs in the body whose primary function is the production of hormones.
Living in groups settled permanently in one place.
A person’s weight in kilograms divided by the square of their height in meters. This is the most widely used measure for identifying obesity. The formula using kilograms and meters (or centimeters) is: weight (kg) / [height (m)]2 . The formula using pounds and inches is: 703 x weight (lbs) / [height (in)]2 . Use of the BMI is controversial for several reasons, including that it does not take into account age, bone structure, muscle mass, fat distribution, or ethnic and racial differences in body type.
The biological system that circulates blood around the body via the heart, arteries, and veins, delivering oxygen and nutrients to organs and cells and carrying waste products away.
A stroke occurs when a blood vessel leading to the brain is blocked or bursts, preventing that part of the brain from receiving blood and oxygen, leading to cell death.
An endocrine disorder in which high glucose (blood sugar) levels occur over a prolonged period of time. Blood glucose is your body’s main source of energy and comes from the food you eat. Insulin, a hormone made by the pancreas, helps glucose from food get into your cells to be used for energy. Sometimes your body does not make enough—or any—insulin (type 1 diabetes) or does not take up insulin well (type 2 diabetes). Glucose then stays in your blood and does not reach your cells.
A hormone produced in the pancreas that regulates the amount of glucose in the blood. Lack of insulin or the inability to absorb insulin causes diabetes.
A system that ranks foods on a scale from 1 to 100 based on their effect on blood-sugar levels. Carbohydrates with a low GI value (55 or less) are more slowly digested and metabolized causing a lower, slower rise in blood glucose and insulin levels.
A predictable response to any significant threat to homeostasis. The human stress response involves the Central Nervous System and the endocrine system acting together. Sudden and severe stress incites the “flight or flight” response from the autonomic nervous system in conjunction with hormones secreted by the adrenal and pituitary glands, increasing our heart rate and breathing and releasing glucose from the liver for quick energy.
The rate at which new cases of a disease occur in a population over a given period of time.
The first occurrence of menstruation.
A cluster of conditions, including increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol levels that occur together, increasing the risk of heart disease, stroke, and diabetes. Lifestyle changes like losing weight, exercising regularly, and making dietary changes can help prevent or reverse metabolic syndrome.
The aggregation (grouping together) of two or more diseases or health conditions in a population in which there is some level of harmful biological or behavioral interface that exacerbates the negative health effects of any or all of the diseases involved. Syndemics involve the adverse interaction of diseases of all types, including infections, chronic noncommunicable diseases, mental health problems, behavioral conditions, toxic exposure, and malnutrition.
Ecological models of health and disease emphasize environmental and policy contexts of behavior, while incorporating social and psychological influences, rather than focusing on individual behaviors. These models encompass multiple levels of influence and can lend themselves to more comprehensive health interventions.
 Baked Potato
Baked Potato Potato Chips
Potato Chips